Connect With Us
Blogs
Blog
Children categories
Plantar Fasciitis: Causes and Treatment
Of the different types of pains occurring in the heel, plantar fasciitis is one of the most common. Its name derives from the area of pain and inflammation: a thick band of tissue called the plantar fascia, which runs across the bottom of your foot. Because the plantar fascia connects your heel bone to your toes, the stabbing pain or deep ache associated with the ailment generally occurs when you take your very first steps in the morning (the “morning hobble”) as the affected foot tries to heal itself in a contracted position through the night.
The pain associated with the plantar fascia normally lessens as your foot limbers up, although it may recur during the day, especially after a prolonged period of standing, or when getting up after having been in a seated position for a while.
Common Causes for Plantar Fasciitis
- Age. Plantar fasciitis is most common in active men and women between the ages of 40 and 60.
- Certain types of exercise. Activities that place repetitive stress on your heel and attached tissue, such as long-distance running, ballet dancing and dance aerobics on hard surfaces, can contribute to an early onset of plantar fasciitis.
- Faulty foot mechanics. Being flat-footed, having a high arch, or even having an abnormal pattern of walking can adversely affect the way weight is distributed when you’re standing and put additional stress on the plantar fascia.
- Obesity. Excess pounds put extra stress on your plantar fascia.
- Occupation. Factory workers, teachers, restaurant servers and others who spend most of their work hours walking or standing on hard surfaces have a higher risk of damaging their plantar fascia.
Importance of Treatment
If plantar fasciitis is left untreated, it may become a chronic condition. You may not be able to keep up your current level and range of activities, and you may even develop symptoms of foot, knee, hip and back problems because plantar fasciitis can affect the way you walk.
How to Cope with Plantar Fasciitis
Home Treatments
- Stay off your feet as much as possible
- Apply ice for 15 to 20 minutes, three to four times per day to reduce swelling
- Reduce or change your exercise routine
- Use arch supports in your shoes
- Do stretching exercises that stretch the Plantar Fascia
- Use anti-inflammatory medication such as Ibuprofen
Medical Treatment
If home treatments fail to bring relief to the plantar fascia, your doctor may opt for an injection of a corticosteroid directly into the damaged section of the ligament, which can help. A procedure that doctors can carry out in their office, they may use an ultrasound device to first determine the best injection site. They may also apply corticosteroids to the skin of your heel or the arch of your foot, followed by a painless electrical current to let the steroid pass through your skin and into the muscle.
Physical therapy can act as ongoing prevention for plantar fascia pain. A physical therapist can also show you exercises to strengthen your lower leg muscles, helping to stabilize your walk and lessen the workload on your plantar fascia.
Prevention for Plantar Fasciitis
To prevent plantar fasciitis, reduce the amount of time spent standing on a hard surface. Exercise on soft surfaces whenever possible, and visit a specialist to make sure you’re wearing the proper shoes for your foot type and gait. It is also beneficial to stretch the plantar fascia regularly. While it’s typical to experience pain in just one foot, massage and stretch both feet first thing in the morning, and three times during the day. It is especially important to stretch adequately before your exercise routine.
Stretching Exercises for the Plantar Fascia
Sit down, and place the affected foot across your knee. Using the hand on your affected side, pull your toes back toward your shin until you feel a stretch in your arch. Run your thumb along your foot–you should feel tension. Hold for a count of 10. Do this stretch first thing in the morning and at least three times during the day and before exercising.
Book an Appointment with Dr. Vikki and Dr. Connie
If you suspect you’re suffering from plantar fasciitis, be sure to get in contact with Dr. Vikki and Dr. Connie. They can help you get to the bottom of your foot pain problem and provide you with the right treatment plan.
Dealing with Ankle Sprains Before They Get Worse
Ankle sprains are very common injuries. Odds are that at some point in every person’s life—be it while running on the playground as a child or landing awkwardly on the stairs as an adult—a sprain will occur. Often sprains are simply complications from over-extended ligaments in the ankle that will clear up on their own. However, in some cases the ligaments will stretch severely or even tear, prompting the need for medical attention.
The most common recipients of ankle sprains are men between the ages of 15 and 24, and women over the age of 30. At least half of all ankle sprains occur during strenuous activity; however, almost as many occur from daily activities such as going downstairs or walking on soft or slippery surfaces. An average of 25,000 people each year seek medical attention for ankle sprains in the United States.
There are a few signs to look out for when sustaining a sprain. With mild sprains there will be pain along the inside of the foot and difficulty walking. Most sprains involve swelling, although with a mild sprain the swelling should not be severe and should go away within a few days. With more severe sprains there will likely be bruising and severe swelling. Most people report a popping or tearing sound occurring at the onset of the injury. It is likely you will not be able to put any weight on the injured foot at all.
The swelling that can occur with a severe sprain is similar to the swelling that occurs with a fracture. It is important to seek medical attention whenever swelling occurs, as there may be a more serious injury capable of worsening if left untreated. Even simple sprains, if left untreated, can turn to joint weakness or stiffness later on.
What Can I Do?
Like many conditions of the foot and ankle areas, there are things you can do at home to lessen the symptoms. The R.I.C.E. method of at-home treatment, derived from the first letters of Rest, Icing, Compression and Elevation, is a useful acronym to remember when dealing with Ankle Sprains.
Rest is generally the first step you should always take after a foot injury. Any amount of weight placed on the affected area can cause severe pain and prompt further injury. It is important to remain off of the affected foot/feet as much as possible, as soon as possible after the injury is sustained.
Icing the affected area for twenty-minute periods is an effective way to minimize the pain and help lessen bruising.
Compression of the injured ankle involves binding the joint with a bandage or boot, which can help to minimize swelling. However, it is recommended that you consult a health professional before binding as further injury can be caused by unskilled methods of compression.
Elevation involves raising the affected foot above the level of your chest, or at least as high as you can safely and comfortably do. This will restrict blood flow to the affected area and decrease pain.
In many cases of a sprain, a boot or crutches will be required to cushion the injured foot or to remove weight from it entirely. Podiatric professionals, like the team at Superior Foot & Ankle Care Center, can help to asses the severity of a sprain and provide the tools necessary to help you heal.
Where Should I Go from Here?
If you have sustained a sprain, chances are that your mobility has suffered. Dr. Vikki and the qualified team at Superior Foot & Ankle Care Center have the tools and training necessary to educate you on how to treat a sprain and how to avoid future injury.
With many years of collective experience, Dr. Vikki and Dr. Connie can help you get back on your feet and stay there. Schedule a consultation today to find out what the team at Superior Foot & Ankle Care Center can do for you!
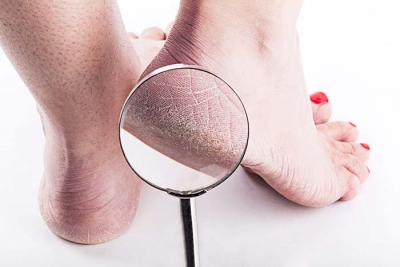
Cracked Feet: Here’s Why Your Feet Are So Dry
Just because your feet are tucked away in socks and shoes for most of the day doesn’t mean that they don’t need moisture, too. If you have noticed cracked heels developing, it’s a sign that the skin on your feet is in dire need of moisture. Left alone, cracked heels can cause pain, bleeding, and even infection.
Cracked heels occur when the skin is too dry to support all of the pressure on it. So when natural expansions of the foot occur during the day, the callused skin on the heel begins to split.
How to Prevent Cracked Feet
- Purchase a good foot cream. Look for rich, heavy moisturizing creams and oils to apply to your cracked feet. Generally, greasier creams works better. Petroleum jelly is a great option if you are unsure where to start. Use the creams (or petroleum jelly) before going to bed, since they take some time to soak in
- Choose your soap carefully. While cracked heels need to be kept clean and dry, harsher soaps will remove too much moisture from your feet. Look for milder soaps or those that note they have moisturizing properties.
- Drink plenty of water. That dry, crackly feeling in your throat when you haven’t had water in a while is indicative of what your skin is feeling, too. Drinking more water will rehydrate your skin and help heal cracked heels.
Believe it or not, the moisture your feet get also depends heavily on how you bathe.
- Moisturize after every shower. Make a point of moisturizing right after a bath or shower to seal moisture in.
- Skip a shower. Bathing more than once a day can actually be harmful for your body. Water from outside the body washes away the oils from your skin and sucks moisture out. The more time you spend bathing, the less moisture your feet retain.
- Set the water to lukewarm. While most people prefer a steamy shower, the hot water will actually dry out your skin. Set the water to room temperature instead.
- Try an oatmeal bath. Bathing with oatmeal-based cleansers are actually a lot less drying than other cleansers, and help prevent cracked feet.
- Don’t scrub your feet. Heavily scrubbing your feet with a towel only dries the skin out even more. Instead, gently pat your skin.
While most cases of cracked heels aren’t serious, soreness, redness, and swelling around the cracked area could be signs of infection and require examination from a podiatrist. If you are worried about infection or simply want to learn more about taking care of your feet, contact Dr. Vikki and Dr. Connie at Superior Foot & Ankle Care Center.
Get the Facts on Foot Ulcers
Foot ulcers can develop into serious wounds and can even lead to the loss of a limb. This is why it is important to adequately treat every cut, callus and blister you sustain because they have the potential to develop into these serious foot ulcers. Here is some information about identifying, preventing and treating foot ulcers.
Who’s at Risk?
People who suffer from chronic illnesses such as sickle cell anemia, nerve damage from alcoholism, atherosclerosis (hardening of the arteries), and those with vascular issues can all be at risk of developing foot ulcers. However, the group that is most at risk are those with diabetes. This is because diabetics often suffer from peripheral neuropathy, which is nerve damage that numbs the extremities to cold, heat and pain.
Because of peripheral neuropathy, diabetics may sustain foot wounds that they are unable to feel and therefore do not treat. Walking around on untreated wounds will often cause them to become foot ulcers. Peripheral neuropathy can also cause the feet to become deformed. Putting deformed feet in normal shoes can cause blisters and calluses that may also develop into ulcers. In addition, diabetics often have poor blood circulation to their legs and feet and, without proper nourishment, the feet are unable to heal themselves of infections.
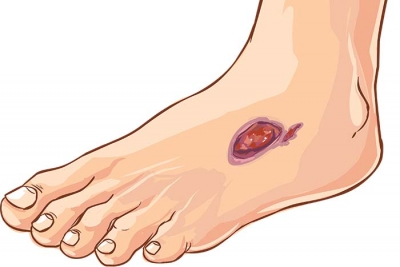
Identifying foot Ulcers
Foot ulcers are red sores found commonly on the balls of the feet or underneath the big toe. If they are infected, they will also produce pus and omit a bad odor. If left untreated, these sores can develop gangrene and your foot will eventually need amputation. For this reason, it is imperative to see a podiatrist if you suspect that you have a foot ulcer so you can be properly diagnosed and treated.
Preventing Foot Ulcers
- Inspect your feet regularly for cuts, blisters and calluses that can turn into ulcers.
- Keep your feet clean and well-hydrated.
- Exercise regularly, this improves your circulation.
- Keep your toenails trimmed properly.
- Don’t go barefoot because it leaves your feet vulnerable to harm.
- Don’t smoke because it weakens your immune system.
Treating Foot Ulcers
Cleansing and Debridement
Your doctor will cleanse the ulcer and remove any dead or dying tissue from the wound. An ointment that promotes healing may be added to the wound before your doctor bandages it.
Stay off Your Feet
Your foot may be put in a cast or protective boot. It is best to stay off your feet as much as possible while you are healing.
Assisted Wound Care
A foot care professional will have to inspect your ulcer once a week until it is fully healed. In addition, a visiting nurse will help dress your wound.
It is critical for diabetics to develop a good relationship with their podiatrists. Most diabetics will require regular care to assure that small problems will not develop into major issues.
Now that you know some facts about foot ulcers, be sure to reach out to a foot care professional if you suspect you have one. If you have any further questions about identifying, preventing or treating foot ulcers or want to book an appointment at the Superior Foot & Ankle Care Center, feel free to reach out to us.
Severe Foot Pain and How to Treat It
Do you have foot pain so severe that it makes it unbearable for you to walk around? Have you tried a bunch of different remedies that just don’t seem to work?
The key to solving your foot pain is first getting the right diagnosis. Here’s a look at some of the common causes of foot pain and how to treat them. However, before you try out any of these treatments by yourself, you should consult with your podiatrist.
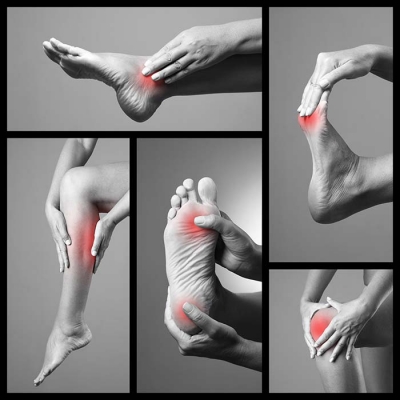
Common Causes of Severe Foot Pain
Your feet carry you around every day, bearing your weight when you’re standing and helping you get to where you need to go. You might not think about your feet too often, that is until they start to hurt. Foot pain is a common problem among people of all ages.
A list of some of the possible causes of foot pain include:
- Achilles tendinitis: is an overuse injury of the Achilles tendon (the band of tissue that connects the calf muscles at the back of your lower leg to your heel bone).
- Bunions: a bony bump that forms at the base of your big toe.
- Bursitis: affects the small, fluid-filled sacs (bursae) that cushion the bones, tendons, and muscles near your joints.
- Corns and calluses: thick, hardened layers of skin that develop when your skin tries to protect itself against friction and pressure.
- Diabetic neuropathy: a type of nerve damage that is the result of diabetes.
- Flatfeet: the entire soles of your feet touch the floor when you stand.
- Gout: sudden, severe attacks of pain, redness and tenderness in joints. Often at the base of the big toe.
- Hammertoe and mallet toe: deformities in the imbalance in the muscles, tendons, or ligaments that normally hold the toe straight.
- Ingrown toenails: when the corner or side of the toenail grows into the soft flesh.
- Metatarsalgia: when the ball of your foot becomes painful and inflamed.
- Plantar fasciitis: pain and inflammation in the thick band of tissue (plantar fascia) that runs across the bottom of your foot and connects your heel bone to your toes.
Treating Severe Foot Pain
Treatments for severe foot pain problems include:
- Achilles tendinitis: usually responds well to self-care measures, such as rest, ice, compression, and elevation; but if your symptoms are severe then your doctor might suggest other treatment options, like pain medications (ibuprofen or naproxen), physical therapy, or surgery.
- Bunions: some nonsurgical options include changing shoes, padding or taping your foot, medications, shoe inserts, and applying ice. Surgical options include removing swollen tissue, removing part of the bone to straighten your big toe, realigning the long bone between the back of your foot and your big toe, and permanently joining the bones of your affected joint.
- Bursitis: treatment usually involves rest, ice, and pain relievers. However, if the bursitis is more severe, treatment might include medication, therapy, injections, an assistive device, or surgery.
- Corns and calluses: treatment options can include trimming away excess skin, callus-removing medication, shoe inserts, or surgery.
- Diabetic neuropathy: treatment focuses on slowing the progression of the disease, relieving pain, and managing complications and restoring function. To help slow the nerve damage you will need to keep your blood pressure under control, follow a healthy-eating plan, get plenty of exercise, maintain a healthy weight, stop smoking, and avoid alcohol.
- Flatfeet: if your flat feet are painful then your doctor might suggest arch supports, stretching exercises, supportive shoes, or physical therapy.
- Gout: medications that can treat gout and prevent future attacks include nonsteroidal anti-inflammatories, colchicine, and/or corticosteroids.
- Hammertoe and mallet toe: wearing proper footwear (allows adequate space for your toes) will help relieve pressure and pain.
- Ingrown toenails: your doctor may recommend lifting the nail, partially removing the nail, or removing the nail and tissue.
- Metatarsalgia: conservative measures (rest, ice, compression, and elevation) usually relieve the pain. In rare cases, you may have to undergo surgery to realign the metatarsal bones.
- Plantar fasciitis: you may be required to take certain medications (ibuprofen or naproxen) and undergo types of therapy (physical therapy, night splints, or orthotics). In some cases, you may have to undergo steroid shots, extracorporeal shock wave therapy, or surgery.
Consult with Dr. Vikki and Dr. Connie
It is important to consult with your podiatrist to make sure that you get a proper diagnosis for your foot pain. Book a consultation with Dr. Vikki and Dr. Connie so that they can help you get rid of your severe foot pain for good.
What Orthopedic Shoes and Inserts Can and Can’t Do for You
At the end of the day, are your feet so sore that you can barely walk? Is this something that occurs on a regular basis? If so, then orthopedic shoes or inserts may be the right solution for you.
But before you run out to the drugstore to pick up some non-prescription inserts, here are some things that you need to know about what orthopedic shoes and inserts can and can’t do for you.
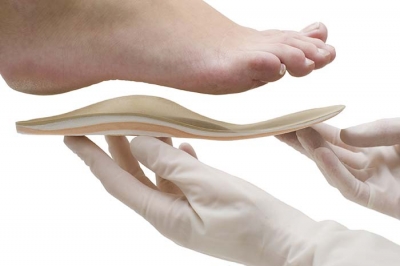
What are Orthopedic Shoes and Inserts?
Orthopedic shoes are specifically designed to provide support and pain relief for people suffering with some type of leg, ankle, or foot pain. While most people tend to think of ugly shoes when they think of orthopedic shoes, today’s orthopedic shoe is a lot more fashion-friendly then they have been in the past, and are worn by people of all ages. The exact design for orthopedic shoes varies depending on the particular health problems of the wearer. There is no one design of orthopedic shoe that will work effectively on all types of foot problems.
Wearing orthopedic shoes is a good idea whenever there is any type of health issue that makes walking painful. All orthopedic shoes and boots share several characteristics, such as:
- Extra firm and low heels
- Wide toes
- Inner soles that can be removed
While the most popular type of orthopedic footwear is shoes and inserts, you can also buy orthopedic socks and slippers.
Prescription vs. Non-Prescription Inserts
Just like orthopedic shoes, shoe inserts can help relieve a variety for ailments, including flat arches and foot pain. Shoe inserts work to cushion your feet, providing comfort and support to your arches. They can also help correct biochemical foot problems or cure long-standing foot issues.
The most common types of shoe inserts are:
- Arch supports: designed to support the foot’s natural arch.
- Insoles: provides extra cushioning and support. They are often made of gel, foam, or plastic.
- Heel liners: also known as heels pads or heel cups. They provide extra cushioning in the heel region.
- Foot cushions: can be used as a barrier to stop your shoe from rubbing against your foot.
Unlike non-prescription inserts, prescription custom orthotics are designed specifically to support and comfort your feet. Prescription orthotics can be divided into two categories: functional orthotics and accommodative orthotics.
Functional orthotics work to treat foot pain caused by abnormal motion and injuries, such as shin splints or tendinitis. Functional orthotics are generally made out of semi-rigid material, like plastic or graphite.
Accommodative orthotics are made out of softer material and are meant to provide additional cushioning and support. They can be used to treat uncomfortable conditions, such as diabetic foot ulcers and painful calluses on the bottom of the foot.
Causes of Foot Pain
Some of the common types of foot pain that orthopedic shoes or inserts can help treat include:
- Plantar fasciitis: irritation or inflammation of the band of tough tissue connecting the heel bone to the toes.
- Heel Spurs: abnormal bone growth on the bottom of your heel.
- Heel fracture: a high-impact injury caused from a fall or car accident.
- Metatarsalgia: pain and inflammation in the ball of your foot.
- Morton’s neuroma: a thickening of tissue around the nerves between the bases of the toes.
- Fallen arches: when the arches of the feet flatten out.
- Bunions: a bony bulge along the edge of the foot, next to the base of the big toe.
- Hammertoe: when your second, third, or fourth toe bends at the middle joint.
- Claw toe: when your toe points up or down and is unable to straighten.
- Sesamoid fracture: a break in the small bones that are embedded in the tendons attached to the big toe.
Book an Appointment
While orthopedic shoes and inserts can do a lot to help your feet feel better, you should make an appointment with a skilled and knowledgeable podiatrist before purchasing your own orthopedic shoes and inserts. Consult with Dr. Vikki and Dr. Connie today about which products will work best for your specific foot needs, and what else you can do to help alleviate your foot pain.
What Causes Your Feet to Make Cracking Sounds?
Do you often find that your feet crack and pop when you’re walking? Are you concerned about what the noises could mean? In most cases, painless cracking and popping isn’t something that you need to worry about. It’s when the cracking causes you pain that you should be concerned.
Here’s a quick look at some of the reasons that might be causing your feet to crack and what it could mean for you.
Painless Cracking
While painless cracking isn’t something that you have to really worry about, you may still be curious about what causes your feet to crack. Some of the things that may cause your feet to crack without causing you pain include:
- Escaping gases—the bones in our joints are surrounded by synovial fluid that lubricates and prevents bones from rubbing against each other. Synovial fluid contains oxygen, nitrogen, and carbon dioxide. When the joint capsule is stretched, these gases form bubbles that cause a popping sound when the bubbles are released. In order to crack the same joints again, you have to wait until the gasses return to the synovial fluid.
- Movement of joints, tendons, and ligaments—the tendon position changes and moves slightly out of place when a joint is moved. This may cause you to hear a snapping sound when the tendon returns to its original position. Also, your ligaments may tighten as you move your joints, which can make a cracking sound.
- Rough surfaces—arthritic joints make sounds caused by the loss of smooth cartilage and the roughness of the joint surface.
Painful Cracking
In some cases, your feet making cracking sounds could be an indication of a greater problem. Some more serious problems that may cause your feet to crack include:
- Morton’s neuroma—a painful condition that affects the ball of your foot, most commonly the area between your third and fourth toes. This condition may feel similar to having a pebble in your shoe. Morton’s neuroma involves a thickening of the tissue around one of the nerves leading to your toes. This can cause your feet to crack, and you may also feel a sharp burning pain, as well as a stinging, burning, or numbing of the toes. This condition can be caused by wearing high-heeled shoes or shoes that are too tight or ill-fitting, causing extra pressure on your toes and the ball of your foot; by participating in high-impact sports that may subject your feet to repetitive trauma; or by foot deformities, such as bunions, hammertoe, high arches, or flatfeet.
- Achilles tendon rupture—the Achilles tendon is a strong fibrous chord that connects the muscle in the back of your calf to your heel bone. Overstretching your Achilles tendon can cause it to tear (rupture) completely or partially. If your Achilles tendon ruptures, you will most likely feel a pop or snap, followed by an immediate sharp pain in the back of your ankle and lower leg. Ruptures tend to occur within two and a half inches of the point where it attaches to the heel bone. It is often caused by a sudden increase in the amount of stress on your Achilles tendon, such as increasing your participation in high-intensity sports, falling from a height, or stepping in a hole.
- Locked joint—if a joint becomes locked when it pops or cracks then there is a chance that something is caught between the joint surfaces. A piece of torn bone or cartilage may be the cause. Once the joint is stuck, it will need to be manipulated to unlock it, which will cause a popping sound.
Book a Consultation
If you experience any pain or swelling in your cracking joints, then it’s important that you seek out medical advice from a qualified healthcare professional. Book a consultation with Dr. Vikki and Dr. Connie today. With years of collective experience in their fields, they’ll be able to help you get to the bottom of what’s causing your feet to make cracking sounds and how the issue can be alleviated.
How Aging Contributes to Foot Issues
Over time, our bodies begin to wear down and our feet are no exception. Myriad changes occur to our feet as we reach our senior years. This includes muscular and skeletal changes, as well as skin and toenail changes, each coming with their own possible challenges. Here is an overview of some of the common foot issues that can come with age:
Changes in Size
Most would assume that shoe sizes stay the same after puberty, but this is not the case. As we age our feet “spread,” which may alter the size of the shoe you should be wearing. Every time you go shopping for a new pair of shoes, you should measure your feet, both for length and width. If it seems like your shoes are growing less comfortable day by day, then you might want to make sure you aren’t outgrowing them.
Skin Issues
One of the more obvious changes we undergo as we age is the thinning of skin. Our feet are no different; and since they are an area that is often subjected to frequent friction, they can see a lot of complications. Due to the weakening and drying of the skin, abrasions are common. Make sure to use moisturizer to keep your skin supple and soft.
Several types of keratosis can make your feet skin look as if it is cancerous or infected, but these raised pigmented bumps are usually benign. Any changes in your skin should be addressed by a physician, as some of these conditions may be masking a more serious affliction.
Arthritis
As the wear and tear on our joints adds up over time, arthritis begins to set in. Arthritis of the feet can be one of the most painful and debilitating forms of this condition, since the feet bear the weight of our bodies. Reduced bone density can also play a role in this type of joint pain.
The weakening of joints and bones can also lead to more frequent fractures and sprains, so it’s important to wear durable, supportive, and comfortable shoes.
Swelling
Circulation problems are also more common with age. Issues with the veins in the legs can cause feet to swell, making shoes ill-fitting from day to day. Sometimes only a single foot will swell, other times both will. Hormonal changes and some medications can be the cause of these issues, as well.
Bunions
An additional reason to wear shoes that fit correctly is bunions. Wearing narrow shoes can cause your big toes to press inwards, jutting out the joint and causing it to elongate and press on the skin. Bunions aren’t only caused by wearing small shoes, as there is also a genetic component to their formation. They can also form on your smaller toes, but they are more pronounced on the big toes.
Hammer Toes
Ill-fitting shoes and arthritis can also cause a condition known as hammer toe. Normally, our toes point outwards from our body, but a hammertoe causes them to point downwards towards the ground. This can affect any toe on the foot, and be quite painful. The physical cause of this downward turn is a dislocation of the middle joint in the toe. Dislocation can be caused by wearing tight shoes such as high heels; or factors such as injury, arthritis, or pressure from the aforementioned bunions.
Gout
A specific type of arthritis, gout is caused by having too much uric acid in the blood stream. While this doesn’t cause symptoms in all patients, in certain individuals these high levels of uric acid cause crystals to form on the joints, usually the big toe. Gout manifests in sudden attacks of pain in the big toe until it is treated. Risk factors for gout include being overweight and having a diet high in meat and alcohol.
Gout is usually somewhat obvious by its visible effects on the big toe, causing swelling and redness. Steroids can stop a sudden gout attack, and there are long-term treatment options as well for chronic gout.
Schedule a Consultation with Dr. Vikki and Dr. Connie
As with any part of the body, investing in your foot health is essential to ensure that your feet age gracefully alongside you. To keep your feet fit for years to come, schedule a consultation with trusted podiatrists Dr. Vikki and Dr. Connie today at the Superior Foot & Ankle Care Center.
Treating Your Foot Rash
Do you have a rash on your feet, but you can’t seem to figure out what’s causing the problem? Not surprisingly, there are many different things that can cause a foot rash to occur, including something occurring near the foot itself or a body-wide condition. A foot rash can affect a small area, be short-lived and mild, or it may spread further up the leg, returning frequently and be painful or itchy. Some foot rashes are also highly contagious.
The first step in treating your foot rash is getting the right diagnosis. Knowing exactly what is causing your foot rash can also help you prevent it from ever returning and turning into a chronic condition. Here’s a look at some of the things that can cause a foot rash, their symptoms, and how to treat them.
Common Causes of Foot Rash
- Irritant contact dermatitis is the most common type of contact dermatitis. Usually caused by damage to the protective outer layer of skin due to contact with chemicals such as household cleaning products, detergents, dyes, cosmetics, or industrial chemicals. This type of rash is not contagious.
Symptoms: Localized dry, cracked, scaly skin, and a non-itchy foot and ankle rash. Symptoms vary depending on exposure to the chemical.
Treatment: Wash the area well, avoid the irritant, use anti-histamines or topical steroids. - Allergic contact dermatitis is caused by exposure to allergens that trigger an immune reaction in the skin. Common allergens include latex rubber, plants, metallic substances, and shoe leather. This type of rash is not contagious.
Symptoms: Pink or red skin with small bumps which may blister. Can be extremely itchy.
Treatment: Avoid the allergen, use a cold compress, anti-histamines or topical steroid medication. - Eczema is a chronic condition that usually starts in early childhood, but can be grown out of. The exact cause is unknown and may be due to a number of different factors, including an inability for skin to provide an effective barrier to allergens, bacteria, and environmental conditions. Eczema can also be hereditary. This type of rash is not contagious.
Symptoms: Dry, red patches of inflamed skin that tend to be itchy (more so at night). Can progress into small, fluid-filled bumps.
Treatment: There is no cure for eczema but you can relieve the symptoms by using corticosteroid cream or ointment, anti-histamines, or UV light therapy. Make sure to regularly moisture the skin, and take shorter, less frequent baths or showers in warm water. - Athlete’s foot is a fungal infection (a type of ringworm) which is often caused by sweaty feet, tight shoes, damp footwear, or anything that makes the foot warm and wet for long periods of time. This type of rash is contagious.
Symptoms: Scaly, itchy, flaky, red foot rash accompanied by a stinging and burning sensation. Blisters may also occur.
Treatment: Anti-fungal medication (usually cream or ointment). Good hygiene such as changing shoes and socks often. - Hand, foot, and mouth disease is a mild viral infection often contracted through coughing and sneezing. This type of rash tends to occur during warmer weather and is highly infectious.
Symptoms: Red, non-itchy hand and foot rash. Blisters may occur in the mouth, hands, and feet. Fever, sore throat, loss of appetite, and a general feeling of being unwell. Dehydration is also a common side effect as it can be painful to drink.
Treatment: Oral anaesthetics and over-the-counter medications (paracetamol and ibuprofen).
Other Causes of Foot Rash
Some of the other, less common causes of foot rash can include:
- Food allergies
- Insect bite or bee sting
- Chickenpox or shingles
- Erythema nodosum (red nodules under the skin)
- Impetigo
- Lyme disease
- Measles
- Mumps
- Rubella
- Roseola
- Scarlett fever
- Meningitis
- Pityriasis rosea
- Rocky Mountain spotted fever
- Strep throat
- Kawasaki disease
- Psoriasis
- Rheumatoid arthritis
- Extreme cold or heat
- Lichen planus (purplish itchy papules)
- Medications
- Stress
- Sunburn
- Allergic purpura
- Anaphylaxis (life-threatening allergic reaction)
Consult with Dr. Vikki and Dr. Connie
Before you try to treat your foot rash at home, it is important to get the right diagnosis to determine the cause of your foot rash. Book an appointment with Dr. Vikki and Dr. Connie today, so that they can help you figure out the best treatment plan for your foot rash.
What Could Be Causing Your Heel Pain?
Do you ever find yourself walking on your toes because it’s too painful to plant your heel? Has your heel been sore for a while, but you just aren’t sure what’s causing the pain? Here’s a quick look at some of the causes of heel pain, why they occur, and how to treat them.
The Most Common Causes of Heel Pain
The most common causes of heel pain are Achilles tendinitis (back of the heel) and plantar fasciitis (bottom of the heel).
- Achilles tendinitis is an injury caused by the overuse of the Achilles tendon (the band of tissue that connects the calf muscle at the back of the lower leg to your heel bone). Achilles tendinitis is caused by repetitive or intense strain on the Achilles tendon; but the structure of the Achilles tendon also weakens with age, making it more susceptible to injury.
Symptoms: The associated pain usually begins as a mild ache in the back of the leg or above the heel after running or other sports activities. More severe pain may occur after prolonged running, stair climbing, or sprinting.
Treatment: Achilles tendinitis usually responds well to self-care measures. However, if your symptoms are severe or persistent, your doctor may suggest other treatment options, such as: over-the-counter pain medications, physical therapy exercises, orthotic devices, or surgery. - Plantar fasciitis commonly causes a stabbing pain that usually occurs with your very first steps in the morning. The pain usually decreases once your foot limbers up, but may return after long periods of standing or sitting. Plantar fasciitis is common in runners, people who are overweight, and those who wear unsupportive shoes.
Symptoms: Pain and inflammation of the thick band of tissue that runs across the bottom of your foot, connecting your heel bone to your toes.
Treatment: Most people can recover with conservative treatments after a few months. In some cases, your doctor may recommend other treatments, such as: pain medications, physical therapy, night splints, orthotics, steroid shots, stem cell injections, or surgery.
Other Causes of Heel Pain
Some less common causes of heel pain include:
- Bursitis is a painful condition that occurs when the bursae (small fluid-filled sacs that cushion the bones, tendons, and muscles near joints) are inflamed.
Symptoms: When the affected joint feels achy or stiff, hurts more when you move it or press on it, or looks swollen and red.
Treatment: Involves conservative measures (rest, ice, and pain relievers). Other treatment options include: medication, therapy, injections, assistive devices, and surgery. - Osteomyelitis is a bone infection that usually affects the feet of people who have diabetes.
Symptoms: Fever or chills; irritability or lethargy (in young children); pain in the infected area; and swelling, warmth, and redness over the infected area.
Treatment: The most common treatment is surgery, followed by antibiotics. Depending on the severity of the infection, surgery may include: draining of the infected area, removing diseased bone and tissue, restoring blood flow to the bone, removing any foreign objects, or amputating the limb. - Peripheral neuropathy is the result of damage to your peripheral nerves that can often cause weakness, numbness, and pain. It can be caused by traumatic injuries, injections, metabolic problems, inherited causes, and exposure to toxins.
Symptoms: Numbness, prickling, or tingling; sharp, jabbing, throbbing, freezing, or burning pain; extreme sensitivity to touch; lack of coordination and falling; and muscle weakness or paralysis.
Treatment: Medications (pain relievers, anti-seizure medications, topical treatments, and antidepressants), therapies (transcutaneous electrical nerve stimulation, plasma exchange and intravenous immune globulin, physical therapy, and surgery), or alternative medicine (acupuncture, alpha-lipoic acid, herbs, and amino acids). - Reactive arthritis is joint pain and swelling triggered by an infection in another part of your body (usually the intestines, genitals, or urinary tract).
Symptoms: Pain, stiffness, eye inflammation, urinary problems, and swollen toes or fingers.
Treatment: Physical therapy or medications, such as: nonsteroidal anti-inflammatory drugs, corticosteroids, or rheumatoid arthritis drugs. - Stress fractures are tiny cracks in a bone that are caused by the repetitive application of force (jumping up and down or running long distances).
Symptoms: Mild or severe pain that worsens over time, and swelling.
Treatment: Reduce bone’s weight-bearing load until the fractures are healed. You may need to wear a walking boot, brace, or use crutches. Surgery may be required, although that is not common.
Contact Your Doctor
The first step to knowing what is causing your heel pain is to consult with an experienced doctor, so that you can get a proper diagnosis. Be sure to consult with Dr. Vikki and Dr/ Connie today. With years of collective experience in their fields, they will be able to help you get to the bottom of your foot pain.
More...
Common Foot Problems that May be Ailing You
Do you feel like there’s something wrong with your foot? It’s sore or itchy, but you just can’t seem to figure out what the problem is. Then it may be time for you to seek counsel from your podiatrist.
But before you book a consultation, here are some of the most common foot problems and what you need to know about them.
Plantar Warts
Plantar warts are hard, grainy growths that tend to appear on the heels or balls of your feet (where you put the most pressure). In some cases, the pressure you apply can cause the plantar warts to grow inward beneath a hard, thick layer of skin.
Plantar warts are caused by an HPV (human papillomavirus) in the outer layer of skin. HPV strains that cause plantar warts aren’t highly contagious, and aren’t easily transmitted from direct contact with another person. They do, however, thrive in warm, moist areas, such as around swimming pools and locker rooms.
Most plantar warts go away on their own, although it might take a year or two. If you find that over-the-counter medications or home remedies aren’t helping get rid of your plantar warts, then you may want to ask your doctor about:
- Stronger peeling medicine (salicylic acid)
- Freezing medicine (cryotherapy)
- Other acids
- Immune therapy
- Minor surgery
- Laser treatment
- Vaccine
Ingrown Toenails
An ingrown toenail refers to a toenail that pierces the flesh of the toe, causing pain, inflammation, or infection. In more severe cases, it can also cause pus and bleeding. Most commonly, ingrown toenails affect the big toe.
There are many things that can cause a toenail to be ingrown, including:
- Your posture
- Your gait
- Foot deformities (bunions, hammer toe, or excessive pronation of the feet)
- Your toenails natural tendency to curl
- Tight footwear, hosiery, or socks
- Not cutting your toenails properly
To prevent ingrown toenails, you must first learn to cut your toenails properly. Cut your nails straight across and don’t cut too low at the edge (the corner of the nail should show above the skin). Cutting your nails after a bath or shower when the nail in much softer can also help. Good hygiene can go a long way in preventing ingrown toenails.
Corns and Calluses
Corns and calluses form when excessive pressure on certain areas of the foot causes skin to thicken as a protective response to the friction of skin rubbing against a bone, shoe, or the ground.
Callus (callosity) is an extended area of thickened skin on the soles of the feet. Calluses are usually caused by an underlying problem (i.e. bone deformity), a particular style of walking, or inappropriate footwear.
Corns are caused by pressure or friction over bony areas, such as joints, and they have a central core that can cause pain if it presses on a nerve. There are five different types of corns: hard corns, soft corns, seed corns, vascular corns, and fibrous corns.
You can treat corns and calluses by occasionally gently rubbing a pumice stone over the tough skin when you’re in the bath. Also, applying moisture cream can help remove the thickened skin a little at a time. However, if you wish to have your corns cut, then you should see a podiatrist.
Athlete’s Foot
Athlete’s foot is a skin fungal infection that can lead to intense itching; cracked, blistered, or peeling areas of skin; redness; and scaling. Large painful fissures can also develop and the condition can spread along all five toes and to the soles of the feet, if left untreated.
Athlete’s foot can be caused by a number of fungal species, which you can pick up from someone else shedding affected skin (usually in places such as pools, showers, and locker rooms) or when you walk around barefoot. Athlete’s foot can also be passed through direct contact with someone who has the infection.
The best way to prevent Athlete’s foot is to make sure your feet are completely dry after washing them, before you put on socks and shoes. It can also help if you rotate between pairs of shoes, since damp shoes can take 24-48 hours to dry.
Book an Appointment
If you are unsure of what problem is ailing your foot, you should book an appointment with a knowledgeable podiatrist. Schedule an appointment with Dr. Vikki and Dr. Connie, so that they can diagnosis your foot ailment and help you get on the right track to having happier, healthier feet.
What’s the Best Way of Dealing with Bunions?
Are you prone to bunions? Maybe they develop because of the shoes you wear or maybe you’re unlucky and they run in your family. Either way, bunions aren’t something that you have to live with forever.
But before you try some drastic home remedy, here’s a quick look at bunions and how to deal with them.
What are Bunions?
The most common type of bunion is an enlargement of the inner portion of the joint at the base of the big toe. This enlargement means that your big toe’s joint is misaligned or that you have an additional bone formation. The misalignment of the big toe causes it to point outward and rotate toward the smaller toes.
A less common type of bunion is located at the joint at the bottom of the pinky toe. This type of bunion is also known as a tailor’s bunion or a bunionette.
Bunions tend to affect a greater amount of women than men. This is most likely a result of the fact that women tend to wear tighter-fitting shoes, which can increase the risk of bunion formation. It has been reported that bunions are more prevalent in people who wear closed shoes than in barefoot people.
Bunions are a progressive deformity and will increase with time, if not properly managed, although the symptoms may or may not get worse.
Causes and Symptoms
Bunions tend to develop when the pressures of bearing and shifting your weight fall unevenly on the joints and tendons in your feet. This shift in pressure causes the big toe’s joint to be unstable, eventually causing the parts of the joint to mold into a hard knob that juts out.
Some of the causes of bunions include:
- Wearing tight shoes and/or high heels
- Inherited (genetic) factors
- Trauma (sprains, fractures, and nerve injuries)
- Neuromuscular disorders (polio or Charcot-Marie-Tooth disease)
- One leg is shorter than the other
- Congenital deformities
While not all bunions cause symptoms, some of the symptoms that bunions can produce are:
- A bulging bump at the base of your big (or little) toe
- Swelling
- Redness
- Soreness
- Thickening of skin at the base of your toe
- Corns or calluses
- Persistent or intermittent pain
- Restricted toe movement
Treatment Options
There are many ways that you can help alleviate the pain of having bunions, all of which can be placed into two categories: conservative treatment and surgical options.
Conservative treatment for your bunions includes:
- Changing shoes
- Padding and taping your foot into a normal position
- Medications (acetaminophen, ibuprofen, or naproxen)
- Shoe inserts
- Maintaining a normal weight through a healthy diet
- Protect the bunion with a moleskin or gel-filled pad
- Wear a splint at night to hold the toe straight
- Use warm soaks, ice packs, whirlpool, ultrasound, and massage
Surgical options include:
- Removing the bump
- Removing part of the bone to straighten your toe
- Realigning the long bone that connects the back of your foot to your big toe
- Permanently joining the bones of your affected joint
Prevention Care
If a diagnosis of your bunion is made early on, it is possible for the bunion’s development to be slowed and, in some cases, stopped with the proper supportive gear. Avoidance of athletic activities with improper shoe fit and toe pressure can also help prevent bunion symptoms to occur.
Some simple ways to help prevent bunions are:
- Wear shoes that don’t cramp or irritate your toes
- Choose shoes with a wide toe (space between the tip of your longest toe and the end of your shoe)
- Your shoes should conform to the shape of your feet without any squeezing or pressing on any part of your foot
- Avoid pointy-toed shoes
- Avoid shoes with heels higher than 2 ¼ inches
Schedule a Consultation
Before trying any conservative methods, it is important that you get a proper diagnosis from your podiatrist to determine what your best options are for dealing with your bunions. Schedule a consultation with Dr. Vikki and Dr. Connie, so that they can help you deal with your bunions properly. With years of collective experience in her field, Dr. Vikki and Dr. Connie are your go-to team in helping you make the right decision about how to get rid of your bunion pain.
How to Deal with Foot Warts
Do you have a wart or warts on your feet, but you don’t know how to get rid of them? You may be surprised to learn that, in most cases, you should be able to treat those pesky warts by yourself. Here’s a quick look at the different types of warts and how you can treat them.
Types of Foot Warts
Warts can occur in a variety of shapes and sizes, appearing either as a bump with a rough surface or as flat and smooth. Some of the different types of warts include:
- Common warts—usually appear by themselves or in groups. They are usually rough, gray-brown, dome-shaped growths. They may also exhibit a cauliflower-like appearance.
- Plantar warts—can develop on any part of the foot. Walking can become painful, and the pressure from walking or standing can push the plantar warts beneath the surface, causing a layer of tough skin similar to a callus to develop over it. Sometimes dark specks are visible beneath the wart’s surface. Multiple plantar warts can form in a large, flat cluster known as a mosaic wart.
- Flat warts—these warts are usually smaller than the eraser end of a pencil, with many occurring in one area. They have flat tops and can be light pink, light brown, or light yellow. Flat warts are often spread by shaving.
- Periungual warts—are rough, irregular bumps found under and around toenails and fingernails.
Home Remedies
Home treatment is often the first treatment for warts, usually proving to be less painful than surgical treatment. Some home remedies include:
- Salicylic acid—this treatment is the most desirable wart treatment because of its effectiveness and safety. It usually takes two to three months.
- Tape occlusion—use duct tape to cover the wart for a period of time. This treatment takes one to two months.
- Over-the-counter cryotherapy—home cryotherapy kits that you can buy without a prescription to freeze away the warts. These kits may be safe for warts on the hands or feet. It is important that you make sure to follow the instructions carefully.
Home treatment for plantar warts differs from treating other types of warts. You can reduce the pain caused by plantar warts by:
- Wearing comfortable shoes and socks
- Avoiding high heels
- Padding the wart with a doughnut-shaped felt or moleskin patch
- Using non-prescription medications (aspirin, ibuprofen, or acetaminophen)
Other Treatment Options
If you find that home remedies aren’t doing the trick with getting rid of your warts, then you should consult with your doctor about cryotherapy.
Cryotherapy is a standard treatment for warts that can be done in a doctor’s office in less than a minute. Cryotherapy involves freezing a wart using a very cold substance (liquid nitrogen), which is usually applied using a probe or a cotton swab. You may have to undergo cryotherapy one to four times, with one to three weeks between each treatment, before your warts go away.
Pain from cryotherapy can last up to three days, although healing is generally quick (seven to 14 days) with little to no scarring. There is also a small chance of infection occurring from cryotherapy.
Wart Prevention
The main way to prevent warts is to avoid contact with HPV (the human papillomavirus). Tips for avoiding HPV include:
- Avoid touching warts on yourself or on others
- Don’t share razors, towels, socks, or shoes with other people
- Avoid walking barefoot on warm, moist surfaces (public showers, locker rooms, or pool areas)
- Keep your feet dry
- Avoid irritating the soles of your feet
Tips on preventing warts from spreading include:
- Keep warts covered with a bandage or athletic tape
- Don’t bite your nails or cuticles
Consult with Your Doctor
It is not odd for people to confuse warts with other skin conditions, such as skin tags or moles, and it is important to make sure that you have a correct diagnosis before you start home treatments. Book a consultation with Dr. Vikki and Dr. Connie so that they can help you get the right diagnosis and the best treatment plan for your foot warts.
Running on Pavement: How Bad Is It For Your Feet?
Any avid runner has weighed in on the debate: which surface is best for running? The science aside, you probably have a personal preference, or are even limited by your immediate surroundings. For many of us, convenience is the deciding factor—and that means running on the ubiquitous pavement of city and suburbia.
While running on pavement poses its unique dangers, you can avoid injury with the right steps and the care of a trusted podiatrist.
The Impact of Running on Pavement
The mechanics of running are complex, with the incidence of injury the result of various factors other than the hardness of the surface you run on. While the jury is still out on whether running on hard surfaces is definitively bad for your feet, it does pose its unique dangers. The two main factors behind the arguments against running on pavement are the negative effects associated with impact and repetition.
Impact: Running is one of the roughest activities our feet can endure. The feet bear up to two to four times your normal body weight while running, repeated up to thousands of times over the duration of your trek. The feet play an integral part in the two essential steps of running: landing and push-off. When running on a hard surface like concrete or asphalt, the ground does not absorb any of the shock of impact upon landing. The weight of impact is then borne fully by the feet, sending vibrations up the leg when landing. When repeated continuously, this process can result in increased injury to the legs and feet.
While running on any pavement is not considered ideal, keep in mind that concrete is considered far worse than asphalt.
Repetition: Citing the aforementioned effects of impact on the feet, repetitive impact causes constant stress to the same muscles and bones in the body, leading to specific injuries. While asphalt would appear to be easier on the body due to its continuous nature, the continuity actually forces the body to endure repetitive trauma to certain muscles. The body is designed to adapt to its surroundings, not bear monotonous stress. Training across various terrains will even out the impact endured while running, lessening the likelihood of injury from repeated trauma.
However, this does not necessarily make running on grass or soil the superior alternative. Softer surfaces like nature trails tend to be more irregular, which is their dual benefit and risk. On one hand, you avoid repetitive impact and injury to the same muscles and bones, which you would suffer on a continuous surface like asphalt. On the other hand, uneven surfaces could present unforeseen obstacles such as pits and dips, resulting in sprains or even broken bones. The best recommendation is to switch up the terrain, to avoid constant impact and injury to certain parts of the body.
Training Tips for City Runners
Regardless of what surface you run on, running injuries are more a function of poor preparation than surface rigidity. A serious runner will know what to expect, and take preventative measures to avoid injury by becoming properly equipped. The first step in this is gaining intimate knowledge of your foot’s unique physiology and its needs, and that starts with consulting a certified podiatrist. Only a trained podiatrist can understand the support demanded by your unique foot anatomy and running patterns, and will advise you on what orthotics and shoes you require to avoid undue foot trauma. Common foot injuries suffered by runners include: plantar fasciitis, heel spurs, stress fractures, and Achilles tendonitis.
Before starting any running regimen, follow these steps:
- Consult your podiatrist. No two feet are the same – not even your feet. Only your podiatrist can identify physical conditions such as fallen arches, or recognize irregularities in your movement patterns such as overpronation. Both require special medical attention to avoid injury when running. In addition to this, no two feet are completely identical, with one possibly requiring extra attention. Consult your podiatrist to determine if you require custom orthotics, supportive inserts, or a specific type of shoe to reduce trauma when running.
- Wear the right shoes. The right equipment is essential to peak performance, and this is especially the case with running. Depending on your running form, you will likely require maximum cushioning and support to reduce the shock of impact, and a flexible sole designed to allow full range of motion. Further specialization is required if your feet overpronate, or if you have wide or narrow feet. Be sure to get shoes designed for the terrain you typically train on, whether it be nature trails or city streets. While running shoes can be extremely expensive, consider it an investment in your foot health.
- Change the terrain. Again, repetitive impact to the same muscle groups can lead to injury. Switching between softer and harder surfaces will allow your body to adapt to different conditions, and provide more comprehensive training to all muscle groups.
Schedule a Consultation with Dr. Vikki and Dr. Connie
To keep your feet in prime shape, schedule a consultation with esteemed podiatrists Dr. Vikki and Dr. Connie today. For all of your podiatric needs, contact the caring specialists at the Superior Foot & Ankle Care Center.