Connect With Us
Blogs

Athlete's Foot (6)
At Superior Foot & Ankle Care Center, we strive to make your podiatric visits as non-scary as possible. Certain foot problems, however, have names that sound quite frightening, but in reality, are fairly common and easily treated. Below are three that might cause you to be alarmed:
Subungual hematomas—not only does this condition sound gruesome, its appearance may give you a scare as well. Its telltale sign is a black toenail. No plague here, however. The black color of the nail is caused by blood pooling under the nail—most often the result of an injury to the toe, like a bad stubbing or a heavy object falling on your foot. Black toenails are also a frequent occurrence among patients who are runners. The repetitive pounding of the toes up against the front of the shoe can result in black nails. In most cases, subungual hematomas will clear up on their own. You might want to get your feet measured to make sure you are wearing shoes that are big enough for your feet.
Onychomycosis—this ten-dollar term is another way of saying you have toenail fungus. Although you may feel that your toe looks like it belongs in a horror movie—discolored, edges that are crumbling and breaking off and odd spots on the nail—fungal nails are often not painful at all. In fact, that’s partly why patients don’t bother getting them evaluated. Fungal infections can spread to other toes and other parts of the body, however, so it’s best to have our podiatrists, Dr. Victoria M. Foley or Dr. Constance Ornelas evaluate a funky looking nail and prescribe the best treatment.
Tenia pedis—you probably know this condition better by its more common name, athlete’s foot. This common foot fungus can be unbearably itchy and cause a red rash, flaky skin and even oozing blisters if left untreated. You get athlete’s foot by coming in direct contact with the fungi and most cases can be prevented by keeping your feet covered in public places and not sharing socks, shoes, or other items that touch another person’s feet.
No matter how bizarre your podiatric symptoms may be, the best course of action is to contact our Long Beach office for an appointment as soon as possible by calling: (562) 420-9800.
You may think you know about athlete’s foot—at least how to recognize it. A red rash that’s dry and flaky and itches and burns like crazy are the telltale signs. However, at Superior Foot & Ankle Care Center we know there’s more to know about this disorder than how it feels. Below are some important facts about this skin condition:
FACT: Athlete’s foot is a fungal infection. There are many different types of fungi that cause athlete’s foot. It’s necessary for our podiatrists, Dr. Victoria Foley and Dr. Constance Omelas to examine your feet and determine the fungus responsible for the outbreak in order to prescribe the correct medicine.
FACT: Athlete’s foot is easily spread to other parts of the body. Fungal toenails and jock itch, for example, can develop when you touch a spot on your feet that has athlete’s foot and then touch someplace else on your body. Athlete’s foot is also extremely contagious to other people.
FACT: Fungi love moist, warm, dark places. Gym locker rooms, the cement around the town pool, public showers, nail salons and the insides of closed-in shoes are all prime spots for fungi to grow.
FACT: You can greatly reduce the risk of getting athlete’s foot if you keep your feet covered when walking in public places and avoid sharing soap, towels, footwear, nail clippers and any other items that touch another person’s foot.
FACT: Personal care habits can also decrease your risk of athlete’s foot. You should wash your feet every day and dry them completely. Using a talcum foot powder on your feet before putting your socks on can help keep feet dry.
FACT: Your footwear choice is important if you are prone to athlete’s foot. Look for socks designed to specifically take moisture away from your feet. Change your socks during the day when you notice that your feet feel moist. Choose shoes that allow air to circulate and feet to breath.
Good podiatric care can help eliminate your chances of getting athlete’s foot. If you have a chronic fungal foot infection problem, contact our Long Beach office (562) 420-9800) to learn ways to get permanent relief.
Did you know that when it comes to self care for patients with diabetes that men are far less likely than women to follow the podiatrist’s instructions? In honor of Men’s Health Month we at Superior Foot & Ankle Center want share some important ways that men (and the women who love them) can greatly reduce their risk of serious diabetic foot complications.
One of the biggest health threats for diabetic patients is an open wound or ulcer. Due to poor circulation and decreased immune system function even seemingly minor cuts or injuries can rapidly become major problems. Infections can develop that are very difficult to heal, leading to serious debilitation and even amputation. To reduce the risk of injury and infection, follow these tips:
Inspect your feet daily: since diabetic patients often have nerve damage which makes it difficult to perceive pain and other sensations, visual examination of the feet becomes very important. If you notice any unusual bumps, red spots, blisters, changes in color, size or shape of the foot you should let our podiatrists, Dr. Victoria Foley and Dr. Constance Omelas know ASAP.
Don’t go barefoot: wearing some type of footwear will reduce the risk of toenail and skin infections since these are transmitted by direct contact. You will also decrease the chances of injuring your foot by banging into something or stepping on a sharp object.
Practice good hygiene: wash your feet daily with warm (not hot) water and a mild soap. Be sure to dry thoroughly, especially between the toes, to help prevent athlete’s foot. Sweat glands can also be affected by diabetes. If feet are dry, be sure to apply a rich moisturizer to prevent cracking. Patients who sweat excessively should use a foot powder to help keep feet dry.
Prevent ingrown nails: keep toenails trimmed short and straight across—curved edges can grow down and back into the skin around the nail bed, opening a doorway for bacteria. If you do develop an ingrown nail, don’t attempt any “bathroom surgery!” Allow the podiatrist to take care of the nail.
Following these simple steps can greatly reduce the risk of disability and health issues from diabetes. If you have questions or are experiencing any unusual symptoms in your feet contact our Long Beach office for an appointment by calling: 562-420-9800.
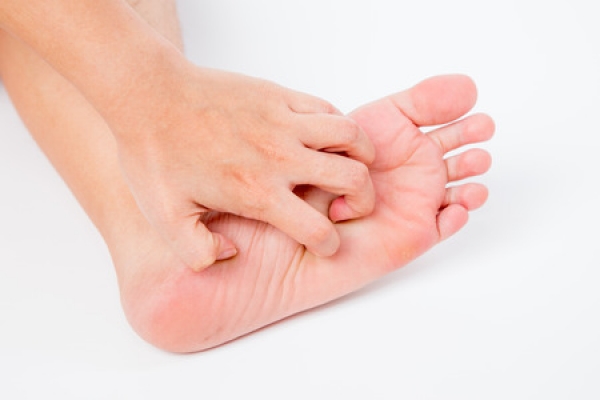
Itchy feet can become the bane of any day: you’re either driven mad trying to resist the urge to scratch; or by the redness, swelling, cracking, and flaking as a result of uncontrollable itching. While the cause could be something benign such as dry skin or excessive sweating, it could also indicate an infection or undiagnosed skin condition. Moreover, if left untreated, other complications could arise, such as a secondary infection.
The itching and burning will only continue to plague you until you accurately identify the source and treat it accordingly. Besides the obvious bug bites or allergic irritation, itchy feet are most commonly caused by a fungal infection or an underlying skin condition. In rare cases, itching could also suggest the presence of another medical condition, such as diabetes. Only examination from a trusted podiatrist can accurately diagnose your foot condition.
Here’s a look at the possible causes of itchy feet, treatment, and prevention tips to keep your feet feeling fresh.
Fungal Infection
When itchy feet are the main symptom, fungal infection is usually the primary suspect: specifically, tinea pedis, or athlete’s foot. Constant exposure to sweat and bacteria, in addition to walking barefoot on contaminated surfaces, make your feet the ideal breeding ground for fungal infection.
Athlete’s foot is an extremely contagious fungal infection which is easily spread through contact with infected surfaces, usually in damp spaces such as showers and gym locker rooms. In fact, it can even be spread through shared towels or linens. The first sign of infection is a dry, scaly rash that causes unbearable itching on the bottoms of the feet and between the toes. While the symptoms can be abated by certain over-the-counter creams, only a podiatrist can effectively cure you of the infection. Once cured, vigilant prevention should be practiced to avoid re-infection.
Skin Conditions
A number of skin conditions can lead to insatiable itching of the feet.
Eczema: Eczema can affect most parts of the body, but dyshidrotic eczema specifically affects the feet and hands. It is characterized by tiny itchy blisters formed on the soles of the feet, which then dry and cause cracking on the skin. If not properly cared for, the exposed skin can become vulnerable to infection. Since dyshidrotic eczema can share symptoms with other skin conditions, a skin sample will likely be taken for proper diagnosis.
Contact dermatitis: Contact dermatitis is a skin irritation that results from contact with an allergen or irritant, which appears similar to a rash. Allergic contact dermatitis is caused by skin exposure to an allergen, triggering an allergic reaction in the affected area. Irritant contact dermatitis is distinct in that it does not involve the immune system, but is instead the result of skin damage caused by exposure to an irritant that rids your skin of its protective surface oils. Common triggers of contact dermatitis include poison ivy, latex, nickel, chemical fragrances, topical medications, and leather.
Psoriasis: Psoriasis is an autoimmune disorder which causes rapid skin cell turnover, resulting in incredibly itchy and scaly dry patches called plaques. The plaques are the result of layers of new skin cells rising so quickly that the dead skin piles atop the surface, rather than gradually sloughing off, form dry patches of thickened skin. Plaques are commonly found on the bottoms of the feet, as well as the elbows and knees.
Additional Sources of Itchy Feet
Here are a few potential, albeit less likely, perpetrators of itchy feet:
- Diabetes: Skin conditions can sometimes indicate diabetes. A condition called eruptive xanthomatosis produces small itchy bumps on the skin as a result of severe diabetes. The condition subsides once the diabetes is managed and under control.
- Scabies: Scabies is an infection of the human itch mite which burrows just below the skin to lay its eggs. The infestation causes intense itching which worsens at night, a pimply rash, and tiny blisters. You can also see traces of the burrows on the skin, which appear as thin whitish lines along the surface. Scabies is easily spread, and should receive medical attention to stem the infection right away.
- Pitted Keratolysis: Pitted keratolysis is a non-contagious bacterial infection, caused by wearing damp, restrictive footwear. It produces shallow pits beneath the toes and soles of the feet, accompanied by itching, burning, and an extremely foul odor.
Prevention Tips
The feet are constantly plagued by bacteria, and need to be cleaned just like your hands. To keep your feet comfortable and fresh, follow these basic hygiene tips:
- Avoid walking barefoot anywhere, especially on damp communal surfaces.
- Always wear dry, clean socks and shoes made of breathable materials.
- Wash your feet thoroughly, and do your best to keep them dry.
- If someone you know has an infection, do not share towels or linens, and protect your feet from contaminated surfaces.
- Keep your toenails trimmed and clean.
If you suspect an infection is already present, schedule an examination with a reputable podiatrist right away.
Schedule a Consultation with Dr. Vikki and Dr. Connie
If itchy feet are wreaking havoc on your life, schedule a consultation with esteemed podiatrists Dr. Vikki and Dr. Connie at the Superior Foot & Ankle Care Center today.
Caring for Your Feet When Training
You’ve decided to start running again. Maybe it’s to lose a few extra pounds or maybe you’re training for a marathon. Either way, it is important to maintain proper foot care to ensure that your feet can carry you the distance.
Here are some quick tips on properly caring for your feet while in training.
Understanding Your Feet
Before you are able to care for your feet, it is important to understand the foot itself. The foot and ankle are complex in structure and mechanics, serving as the foundations for your body with shock absorbing properties.
The foot and ankle contain 26 bones (25% of the body’s bones), 33 joints, more than 100 muscles, tendons, and ligaments. The foot can be divided, anatomically, into three parts: forefoot, midfoot, and hindfoot.
- Forefoot—consists of five toes and their connecting bones. The toes are connected to the metatarsals by five joints at the ball of the foot. The forefoot balances pressure on the ball of the foot, bearing roughly half of the body’s weight.
- Midfoot—forms the foot’s arch, serving as a shock absorber. The bones in the midfoot connect to the forefoot and hindfoot by muscles and the arch ligament.
- Hindfoot—is made up of three joints which link the midfoot to the ankle. The heel bone is the largest bone in the foot, and underneath that bone is a cushioning layer of fat.
Tips on Proper Foot Care
- Invest in proper running shoes—it is important to have your feet properly measured or fitted for shoes that meet your needs. Some people require less support, while others need more cushioning. If you require a shoe that is out of the ordinary, you should try shopping at a specialty running store.
- Wear the right shoes when you aren’t running—the shoes you wear when you aren’t running matter just as much as your running shoes. High heels are the worst type of shoe that a female runner can wear because they push your center of mass forward, throwing off your hip and spine alignments. Modifying your heel-wearing time will reduce aches and may even improve your running form by reducing calf and foot tightness.
- Invest in high quality socks—ill-fitting and non-wicking socks are one of the top causes of blisters. A poor fitting sock will allow your shoes to rub against your heels, which can cause a lot of pain while you run. Non-wicking socks don’t let your feet breathe, creating a wet environment when you sweat, which could lead to athlete’s foot and foot fungus.
- Get stronger—performing barefoot exercises will ensure that every muscle and ligament in your lower body is in working order. You should try to add strength work into your training two or three times a week. The key is to include exercises that improve mobility and balance. Yoga and Pilates are a great way to strengthen and stretch the feet.
- Fix your form—increasing your cadence will help improve your running form. A slow cadence likely means that you’re covering too much ground with each step, increasing the impact forces on your body. Do a quick inventory of how often your foot hits the ground by counting the number of steps taken by one foot for one minute. If you have less than 88 strides, then your cadence is too slow.
- Soften your skin—most runners tend to have dry feet, which can lead to painful cracking. Moisturize your skin every day, rubbing the lotion in until your feet feel soft and smooth.
- Cool down your toes—if your feet swell or get overheated when you run, you should consider applying ice or soaking your feet in cold water right after your run. Elevating your foot above your chest will also help reduce swelling.
- Massage—while massaging your own feet might not be quite the same as having someone else do it for you, it can still be quite effective. You should start by rubbing your feet for several minutes before dusting them with foot powder. Then continue to rub your feet until they feel smooth.
Schedule an Appointment
If you feel any discomfort after running or even after a long day spent on your feet, then you should schedule an appointment with Dr. Vikki and Dr. Connie. With years of collective experience between them, they will get to the bottom of what’s causing your foot pain and map out the best solution for you.
What is Athlete’s Foot?
Athlete’s foot is a fungal infection caused by the tinea fungus, and is usually found between the toes. Its medical name is tinea pedis– ringworm of the feet. It most commonly affects those who are highly active, and thus prone to having sweaty feet confined within tight shoes often and for extended periods of time.
Athlete’s foot is not only embarrassing, but highly contagious. The infection can spread via contaminated surfaces such as floors and laundry. If not careful, the infection can also spread to other parts of the body, such as the hands, nails, and groin.
Learn more about the symptoms of athlete’s foot, and how to prevent an infection of your own.
Athlete’s Foot Symptoms
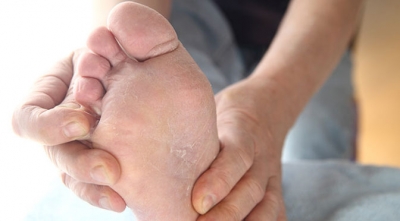
The visual indication of an athlete’s foot infection is a red rash between the toes that is scaly in appearance, with some occurrences even presenting blisters or ulcers. This rash causes the sensations of itching, stinging, and burning. The itching is usually most intense immediately after removing the socks and shoes.
You may also experience dry, cracked, raw, or peeling skin between the toes and on the soles of the feet. Thick, discolored toenails detached from the nail bed are another indication of an infection.
Some strains of the tinea pedis fungus can cause chronic dryness and chafing on the soles and sides of the feet. This can often be mistaken for other skin conditions such as eczema. The infection can spread to other parts of the body, such as your hands, if you pick at the infected sites.
Causes & Risk Factors
Athlete’s foot is closely related to ringworm and jock itch, and is actually caused by the same fungal infection. The tinea pedis fungus thrives in warm, damp environments, making sweaty socks the perfect incubator for its growth. It is most commonly found in moist public spaces, such as communal locker rooms, public showers, gyms, and swimming pools. Walking anywhere barefoot is highly discouraged.
Certain environmental factors put you at higher risk of contracting an athlete’s foot infection. For one, males are more likely to develop the infection. If you are highly active, meaning that you wear sweaty socks for extended periods of time, then you are at higher risk. Since the fungus is highly contagious, being exposed to an environment such as a communal gym or shower with an infected individual makes you extremely likely to catch the infection. Moreover, if you share a home with someone who is infected, you may catch the infection through contaminated floors, shared bedding, shared towels, etc. For this reason, those who tend to walk barefoot in public spaces are at a higher risk. This includes those with compromised immune systems, such as those with diabetes.
Athlete’s Foot Diagnosis
An experienced podiatrist can often diagnose an athlete’s foot infection through visual confirmation. However, he or she may also take skin samples to view under a microscope or send to a lab for testing for a definitive diagnosis.
Common tests include:
- PAS stain
- Skin culture
- Skin biopsy
Athlete’s Foot Treatment
Athlete’s foot is similar to other common fungal infections, and mild cases can be treated with over-the-counter antifungal medications such as creams and ointments. Over-the-counter antifungal medications include: Lamisil AT and Lotrimin AF.More serious cases may require prescription medication to be applied topically to the feet. For the most severe cases, your doctor may prescribe oral antifungal pills to flush out the infection. Common oral antifungal prescriptions include: Sporanox, Diflucan, Gris-Peg or Lamisil.
At home, you may soak your feet in salt water to help remedy the blistering. Tea tree oil is also a common natural remedy used with some limited success. Of course, only a doctor’s visit can be trusted to completely eliminate the infection.
Prevention
The most effective treatment for any infection is prevention.
- Avoid walking barefoot in any public space, especially ones that are humid and moist such as a locker room.
- If you know that a family member has contracted the infection, do not walk barefoot on any communal floors, and refrain from sharing linens such as bedding and towels. Even try to use different showers until the infection clears, if possible.
- Wash your feet thoroughly with antibacterial soap, and dry them fully.
- Apply antifungal powders daily, if necessary.
- Wear socks with breathable fibers such as cotton or wool, or specially designed moisture-wicking features.
- Change your socks as often as possible, and alternate between different pairs of shoes to allow them to dry out between uses.
- If the infection seems unavoidable due to a highly active lifestyle, seek treatment at the first signs of infection to avoid it from spreading to the hands, nails, or groin.
- Seek medical attention immediately if you have diabetes or compromised immune health.
Potential Complications
The fungal infection can potentially spread to your hand, your nails, and your groin (jock itch).
You may also develop an allergic reaction to the fungus, resulting in blistering on the affected area. Moreover, an additional bacterial infection may develop. A bacterial infection may also be present if your foot becomes painful and swollen, or if it develops pus and drainage. Seek medical attention if you develop a fever to prevent the infection from spreading throughout the body.
Consult Esteemed Podiatrist Dr. Vikki
If you suspect that you may have an athlete’s foot infection, schedule a consultation with podiatrist Dr. Vikki today. Dr. Vikki is a diplomat of the Board of Podiatric Surgery, and the trusted podiatrist of the Special Olympics. Just look to her well-earned reputation for excellence in patient care. For all of your podiatric questions and concerns, contact the specialists at the Superior Foot & Ankle Care Center.