Connect With Us
Blogs

Foot Conditions (12)
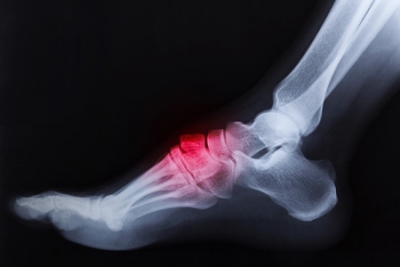
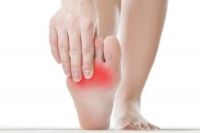
At Superior Foot & Ankle Care Center we know that pain at the back of your heel can be quite debilitating. What starts as an annoying ache can quickly turn into excruciating pain that makes walking difficult. For our Los Angeles County patients that may be experiencing these uncomfortable symptoms, here are three possible causes.
Haglund’s Deformity—this is a bony enlargement that forms at the back of your heel. This condition may be the result of an inherited structural issue like a high arch or a tight Achilles tendon. It can also be caused by wearing shoes with stiff backs that rub on the heel—hence this deformity’s other name: pump bump.
Bursitis—small sacs that are filled with fluid—known as bursas—are found throughout the body near joints and bones. They serve as protection from friction and provide a little extra lubrication. When a bursa becomes irritated due to repetitive motion or pressure it can become painfully inflamed. Haglund’s deformity is one cause of bursitis but it may also be the result of repetitive action from exercise or another medical condition such as gout, diabetes or arthritis.
Achilles Tendonitis—this long tendon that runs down the back of your lower leg connects your calf muscle to the heel bone. It can be aggravated or injured from overuse such as someone whose job involves climbing a ladder. Athletes and “weekend warriors” who suddenly increase the intensity of their workout routine may also suffer from Achilles issues.
The only way to find out for sure what’s causing your back of heel pain is to let our podiatrists, Dr. Victoria M. Foley and Dr. Constance Ornelas, examine your foot and conduct the necessary tests to get to the bottom of the problem. You can contact our Long Beach office at (562) 420-9800 office for an appointment. To learn more about foot health and conditions we treat check out our video library.
At Superior Foot & Ankle Care Center we thought we’d get into the spirit of Halloween for our Los Angeles County patients by exploring some foot problems that have frightening names. If our podiatrists, Dr. Victoria M. Foley and Dr. Constance Ornelas told you that you had one of the disorders named below, you might panic. But in reality, these are just the medical names for some fairly common and easily treatable conditions. And, our friendly podiatrists would most likely tell you the “user-friendly” name of your foot problem to avoid alarming you!
Tinea Pedis—You’d probably be less scared if you heard “athlete’s foot,” the common name for this itchy skin problem. Often beginning between your toes, the skin will be red, itchy, and flaky. In advanced cases, oozing blisters and cracks in the skin may develop. There are a number of topical treatments that the foot doctor may prescribe to eliminate athlete’s foot. Of course, it’s better to avoid contracting it in the first place. To prevent athlete’s foot, wear shower shoes when walking in public places like community pools and gyms, avoid items that touch another person’s foot, and keep feet dry.
Medial Tibial Stress Syndrome—You may experience this podiatric problem if you’ve recently started a new walking or running program. Its shorter name is “shin splints.” Telltale signs include pain, swelling, and tenderness in the front of the leg on either side of the shin bones. It’s important that you have your legs and feet examined by the foot doctor if you have shin splints because there are a number of different causes of this condition. Left untreated, the pain will get worse and may even lead to a stress fracture.
Onychomycosis—What does it mean when your toenails become discolored and get thick and crumbly? Most likely you’ve contracted toenail fungus—also known as onychomycosis. Fungal toenails are harder to get rid of than other fungal infections. The foot doctor will prescribe the best treatment option for you. We also offer KeryFlex Nail Restoration System to repair nails damaged by fungal infections.
We don’t ever want any of our patients to be fearful about seeing the podiatrist. If you notice anything that looks even a little frightful about your toes, feet or ankles make an appointment at our Long Beach office today by calling: (562) 420-9800.
At Superior Foot & Ankle Care Center we see patients whose symptoms don’t immediately point to the cause of the problem. Flatfeet can be one of those conditions. Patients with flatfeet may experience one or all of the following symptoms:
- Pain in the foot, ankle, heel and/or lower leg
- Lack of flexibility in the foot
- General aching or fatigue in the foot or leg
- Swelling in the midfoot area
- Overpronation
- Shin splints
- Lower back, knee or hip pain
Finding the Cause
There are several types of flatfeet. They share one defining characteristic: a partial or total collapse or loss of the arch of the foot. Some possible causes of flatfeet include:
- Heredity
- Abnormal development of the arch during childhood
- Trauma or injury
- A gradual loss of arch over time due to aging, weight gain or medical conditions such as arthritis
This deformity may be present in varying degrees and therefore result in varying severity and kinds of symptoms. If you are experiencing any of the above symptoms, it’s a good idea to make an appointment at our Long Beach office so that our podiatrists, Dr. Victoria Foley and Dr. Constance Omelas can examine your foot.
To diagnose flatfoot, the foot and ankle surgeon will examine your foot and observe how the arch looks when you are standing and sitting. Most likely x-rays will be ordered to determine the severity of the deformity.
Treatment Options
How to best treat flatfoot will depend on how advanced your condition is and the symptoms you are experiencing. Some patients with flatfoot experience no symptoms and the foot doctor may just advise you on ways to prevent worsening of the flatfoot and what you can expect in the future. For those with symptoms, a number of non-invasive treatments exist including modifying your footwear, using custom orthotics, and physical therapy.
If you believe you may have flatfeet, contact us for an evaluation today by calling: (562) 420-9800.
A condition that we see frequently at Superior Foot & Ankle Care Center is flat feet. True to its name, “flat feet “describe a deformity in the foot where the arch of the foot is virtually nonexistent when a patient is standing. Although for many patients flat feet are not initially painful, they can lead to pain in the ankle, lower leg or middle of the foot. Having flat feet also makes you more susceptible to some other foot conditions such as plantar fasciitis. In addition to pain, flat feet can cause swelling and a lack of flexibility in the foot.
Who Gets Flat Feet?
There are several possible causes of flat feet. For some patients, the arch of the foot fails to develop properly during childhood. In other cases, it is something that occurs over time as the result of risk factors such as:
- Heredity
- Trauma or injury
- Aging
- Weight gain or pregnancy
- Arthritis
What Can be Done?
The course of treatment for flat feet will depend on the severity of the symptoms. Whether you have pain or not, if you notice that your feet seem to be flat and the floor without a normal arch you should contact our Long Beach office so that our podiatrists, Dr. Victoria Foley and Dr. Constance Omelas can examine your feet. Due to the possible genetic component of the condition, the foot doctor will want to get a family medical history as well. At the very least, the podiatrist will want to monitor your flat feet to ensure that a progressive disability does not develop over time. If you do have stiffness or pain the foot doctor may suggest any or all of the following:
- Stretching
- Physical therapy
- Icing
- Using arch supports or foot braces
If conservative measures don’t work or the arch issue is severe, reconstructive surgery may be an option.
If you have questions about flat feet or want to make an appointment to have your arches evaluated call us at 562-420-9800. We offer appointments before and after work and our helpful staff will work with you to find a time that works best with your busy schedule.
With approximately 25% of all the bones in your body residing in your feet, fractures are an important concern here at Superior Foot & Ankle Care Center. A general fracture, one that goes all the way through a bone, usually occurs as the result of an accident or other trauma and is immediately apparent. There is a second kind of fracture, however, that is not always so obvious: a stress fracture. Stress fractures are tiny fissures or cracks in the surface of a bone. They typically occur in the area from the middle of your foot extending to your toes, also called the forefoot.
Symptoms of a stress fracture are similar to those of a general fracture:
- Pain
- Swelling
- Bruising at the site of injury
- Tenderness
- Difficulty bearing weight on the affected foot
The difference, however, is in the way the symptoms present. Often with a stress fracture the discomfort will be intermittent; worse when you are active and on your feet and better when you are resting your foot. That’s why it’s important to make an appointment at our Long Beach office if you experience any of the above symptoms even if they don’t seem very intense. Our podiatrists, Dr. Victoria Foley and Dr. Constance Omelas will be able to determine if you have a stress fracture or if your symptoms are due to another condition.
One important way that you can help prevent stress fractures is by making sure that you have an adequate intake of vitamin D. Although calcium seems to get all the credit when it comes to bone strength, it’s actually vitamin D that enables your body to absorb and regulate the calcium.
Many people have a vitamin D deficiency and don’t even realize it. Vitamin D deficiencies are more common if you have one or more of the following factors:
- Being over 50
- Limited sun exposure (the sun being a good source of vitamin D)
- Dark complexion
- Overweight
- A medical condition that causes fat malabsorption
Your doctor can do a blood test to check your vitamin D levels.
Other ways to help prevent stress fractures include avoiding injury and repetitive activities that put pressure on the forefoot. If you believe you may have a stress fracture contact us by calling: 562-420-9800.
At Superior Foot & Ankle Center we find that many patients do not fully realize the role the podiatrist can play in your foot and overall health. Our purpose is to provide acute and preventive care to your entire lower extremity (from the tips of your toes up to your knees). We have a wealth of treatment options available including pain relief, multiple therapies, custom orthotics, exercise and surgery to correct and improve foot discomfort associated with both age and activities, including sports injuries. In addition, in many cases the foot doctor is able to diagnose a larger, systemic issue from symptoms in your feet and can then collaborate with other health care professionals to care for the disorder.
Use the following as a guideline if you’re trying to decide if you should call the podiatrist:
- You experience sudden or increasing pain; chronic pain seems to be getting more severe or more frequent
- You notice abnormalities in your feet: swelling, changes in shape or size, bruising, lumps,
- Other non-painful symptoms: tingling, burning, itching, pins and needles, numbness
- Changes in skin (color, redness, scaling, flaking, sores, blisters, cracking) or toenails (discoloration, thickening, crumbling, peeling)
- Possible signs of infection: pus or discharge, redness or red streaks, tenderness, heat, fever
- You have any symptoms and have diabetes or other conditions that suppress the immune or circulatory systems—even the most minor symptoms can become major medical threats to these patients
If you said yes to any of the above symptoms or signs, contact our Long Beach office for an appointment by calling: 562-420-9800. Our foot and ankle surgeons, Dr. Victoria Foley and Dr. Constance Omelas will do a complete examination and help get to the bottom of your foot pain so that you can get back to the active lifestyle you love. Regardless of whether your foot disorder is common, such as athlete’s foot or an ingrown toenail or a more complex condition, starting treatment sooner rather than later will enable the foot doctor to use the least invasive methods and ensure the quickest cure.
Although the risk for athlete’s foot is high during the summer due to the fact that patients go barefoot more often in public places, at Superior Foot & Ankle Care Center we see just as many cases as we move into the fall. Part of the reason for this is that the fungi that causes this infection (also known as tinea pedis) love warm, moist, dark places—like inside closed shoes and sweaty socks.
How do You Know if You Have It?
The symptoms of athlete’s foot are severe itching, burning and redness, along with dry scaly skin. The infection often begins between the toes but can also develop on the arches, soles or the sides of the feet. Left untreated, blisters may form and the condition can progress from annoying to painful. What’s tricky, however, is that the symptoms of athlete’s foot can mimic other conditions, such as psoriasis. In addition, there are different fungi that cause athlete’s foot, which may affect treatment. For those reasons, it’s important to get a skin rash on your foot looked at sooner rather than later. Our podiatrists, Dr. Victoria Foley and Dr. Constance Omelas will examine the skin on your feet and make an accurate diagnosis of the condition.
Treatment and Prevention
Both topical ointments as well as oral medications are available to treat athlete’s foot. The foot doctor will prescribe the treatment that will be most effective depending on the type and severity of your infection. Of course, the best scenario is not to get athlete’s foot in the first place! Some tips for avoiding athlete’s foot include:
- Do not share shoes, socks, towels or any other items that touch another person’s feet.
- Keep your feet from coming in contact with fungus by wearing shower shoes or flip flops in gyms, locker rooms, showers and other public places where people walk barefoot.
- Keep feet dry. Change your socks more than once a day if you tend to perspire heavily.
- Wash feet daily and dry completely, being sure to get the space between the toes. Apply a foot powder before putting on socks to help keep feet dry.
If you are concerned that you may have contracted athlete’s foot, contact our Long Beach office for an appointment by calling: 562-420-9800.
Chances are if you haven’t had sesamoiditis, you may not have any idea what it is. However, at Superior Foot & Ankle Center we often find that for patients suffering from pain in the ball of the foot, sesamoiditis is the cause.
What are Sesamoids?
Sesamoids are a unique structure in the body. They are tiny bones that are embedded in a tendon and are not connected to other bones. They are only found a few places in the body and your feet are one of them. Two sesamoids are located on the bottom of your foot at the base of the big toe. They act kind of like pulleys in the tendon, enabling it to move more easily and helping the big toe with pushing off.
Too Much Pressure
Due to their location and function in the foot sesamoids are exposed to excessive amounts of pressure and force. They can become over stressed or even injured from activities such as running and other sports, dancing, jobs that require you to be on your feet all day and having high arches or wearing high heels frequently. When the sesamoids become inflamed and irritated that is the condition of sesamoiditis.
Diagnosis and Treatment
In addition to pain in the ball of the foot, patients with sesamoiditis may also experience pain at the base of the big toe as well as swelling and bruising in that area. The big toe may be stiff and difficult to bend. Our podiatrists, Dr. Victoria Foley and Dr. Constance Omelas, will want to examine your foot, paying particular attention to the big toe. Digital x-rays (which can be done right in our Long Beach office) and other imaging studies may be needed to confirm the diagnosis.
There are a number of treatment options available for sesamoiditis, depending on the extent of the condition, including:
- Over the counter anti-inflammatory medications or steroid injections to help reduce pain, swelling and inflammation
- Bracing, taping or strapping the toe to relieve pressure and allow healing
- Wearing soft-soled, low-heeled, cushioned footwear.
- Orthotics
- Physical therapy
If you are experiencing symptoms of sesamoiditis, stop any activities that cause pain and contact us for an appointment by calling: (562) 420-9800.
Pump Bump is the common name for Haglund’s Deformity. Many patients that we at Superior Foot & Ankle Care Center see with this condition mistakenly believe that it is caused by their shoes. In reality, the bony protrusion at the back of the heel is the result of faulty foot structure which is often inherited. Other conditions that can lead to pump bump include:
- Underpronation (walking on the outside edge of your foot)
- High arches
- Tight Achilles tendon
Reducing Pain and Irritation
Our podiatrists, Dr. Victoria Foley and Dr. Constance Omelas, will need to examine your foot to confirm a diagnosis of Pump Bump. The foot doctor will likely order x-rays of the back of the heel as well to evaluate the bone structure and rule out other conditions that might cause pain and irritation in that part of the foot.
Shoes with stiff backs that repeatedly rub against the bump make it red and painful. Pumps consistently hit the spot where the deformity is located and hence the name, Pump Bump. Other shoes are problematic also, including high topped work boots, ice skates and certain men’s dress shoes. If you have Haglund’s Deformity you obviously have to be selective about your footwear. A callus or open sore can form if you continue to wear shoes that put pressure on this spot.
There are several other ways to relieve the pain and decrease the friction on the bony enlargement, depending on what else is putting stress on the back of the heel. The foot doctor may recommend heel lifts to help compensate for high arches, stretching exercises if you have a tight Achilles tendon, or custom orthotics to help control the motion of the foot. Padding, immobilization and medication are other avenues of treatment. If you continue to be in severe pain despite these noninvasive measures, surgery may be required.
The bottom line is if you have Pump Bump you don’t need to continue to suffer. Make an appointment at our Long Beach office by calling 562-420-9800 and find out what can be done to relieve your painful symptoms.
Our feet are pretty forgiving. They take us where we need to go and help us stay fit by enabling us to participate in sports and exercise activities. They even accept being crammed into uncomfortable shoes now and then for the sake of fashion. However, we can push it too far. When an excessive amount of pressure is put on our feet we are susceptible to many foot disorders. One of them is metatarsalgia. This condition’s telltale sign is pain in the ball of the foot where the five long metatarsal bones end. At Superior Foot & Ankle Care Center we find that there are many ways that patients put too much pressure or uneven pressure on this part of the foot, including:
- Standing or walking for long periods of time on very hard floors or ground
- Frequently participating in weight-bearing activities such as running, dancing or basketball
- Wearing shoes that fit improperly or spending too much time in shoes with very rigid soles such as work boots or hiking shoes
- Gaining weight
Sometimes, metatarsalgia is caused by conditions that are beyond a patient’s control such as arthritis, flatfeet (overpronation), an injury or foot deformity. This condition is also more likely to occur with age as the fat pads on the bottom of our feet naturally begin to wear down.
Treating Metatarsalgia
If our podiatrists, Dr. Victoria Foley and Dr. Constance Omelas, diagnose metatarsalgia the first step will be to reduce the pain and discomfort that you are experiencing. This can usually be accomplished with rest, icing and anti-inflammatory medications. The next step will be to deal with the root cause of the condition. Depending on what the source of foot pressure is, the foot doctor may recommend changing the types of shoes you wear, losing weight, treating an existing condition or using a custom orthotic device to alleviate inflammation to the affected area.
Be good to your feet by not waiting to seek medical treatment if you are experiencing pain, discomfort or other unusual symptoms. Contact our Long Beach office for an appointment by calling: (562) 420-9800.
More...
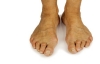
One thing just about everyone knows about hammertoe is how to recognize it. The telltale downward bend of the toe in the shape of a hammer make it an obvious deformity to spot. At Superior Foot & Ankle Care Center we have found that beyond its appearance, many patients don’t have all the facts about this condition. Below are some common questions and answers about hammertoe:
- What’s the cause of hammertoe? This condition is often the result of a muscle imbalance but can be exacerbated by wearing shoes that don’t fit well or styles that have narrow toe boxes or force the foot into the front of the shoe, like high heels. Other possible factors in a hammertoe forming are genetics and arthritis.
- Which toes are affected? The second, third and fourth toe are usually the ones affected by this condition.
- Is all the pain and discomfort in the joint? No. While the abnormal position of the toe does cause inflammation, pain and discomfort, corns often form on the top of the toe due to the friction of rubbing on shoes and calluses may develop in the ball of the foot from the excessive pressure caused by the bent toe.
- How are hammertoes treated? Treatment of hammertoe is multi-dimensional. Our podiatrists, Dr. Victoria Foley and Dr. Constance Omelas will want to perform a complete examination of your toes and feet, which may include x-rays. If you are experiencing a fair amount of pain, anti-inflammatory medications and cortisone injections may be recommended to reduce the pain and inflammation. To correct the hammertoe, custom orthotics and/or splinting and taping the affected toe may be an option. Physical therapy and exercise can help stretch and strengthen the toe.
- Will hammertoe go away without treatment? Hammertoe is a progressive condition. In fact, if left untreated, the toe will become increasingly rigid in its bent position and eventually will only be correctable with surgery.
If you have noticed any signs of hammertoe, the sooner you get it evaluated the less intense and more successful non-surgical treatment is likely to be. Contact our Long Beach office for an appointment by calling: 562-420-9800.
A common condition that we treat at Superior Foot & Ankle Center is the bunion. A bunion, also known as hallux valgus, is an enlargement of the joint at the base of the big toe which forms when the bone of the joint moves out of place and toward the second toe. The further the toe moves the more the framework of the foot becomes deformed and the bigger the bump that forms on the outside of the toe grows. Bunions can cause considerable pain due to all the weight and pressure put on the big toe as you walk and also from the friction that occurs from shoes rubbing on the protrusion. Other symptoms include inflammation and redness, a burning sensation and numbness. Bunions are progressive. Over time, corns or calluses may form on the toe and the range of motion may become limited.
What’s Behind a Bunion?
Bunions form as a result of an abnormality in the structure of the foot which shifts the forces exerted on the joints and tendons in a way that causes instability and ultimately deformity of the joint. Possible reasons for this include:
- Inherited faulty foot mechanics
- Neuromuscular disorders
- Consistently wearing shoes that have narrow toe boxes and/or are too small, squeezing the toes together in an unnatural position
Treatment and Relief
Many people suffer unnecessarily with bunions. It is true that when bunions are severe and causing serious disability and pain that surgery may be needed to remove the bony enlargement and correct the alignment of the toe joint. Before reaching that point, however, there are several conservative treatment options available, including:
- Changing to shoes with wide toe boxes and avoiding high heels
- Padding and/or taping the toe to reduce pain and keep the toe in its correct position
- Ice packs, anti-inflammatory medications and cortisone injections to lessen pain and inflammation
- Custom orthotic inserts for your shoes to correct toe alignment and take pressure off the painful area
You won’t know what relief is available until you have one of our podiatrists, Dr. Victoria Foley and Dr. Constance Omelas examine your bunion and determine its severity. If you are suffering with bunion symptoms, contact our Long Beach office by calling 562-420-9800 for an appointment today.