Connect With Us
Blogs
Displaying items by tag: Foot Doctor
Celebrating National Nutrition Month
At Superior Foot & Ankle Care Center, we know there’s a direct connection between what you eat and your feet. Eating a well-balanced and nutritious diet can positively impact your podiatric health in several ways:
- Decreasing the amount of foot pain you experience by helping you attain and maintain a healthy weight
- Lower your risk for developing many lower extremity disorders like flat feet, sesamoiditis, heel pain and more
- Reducing inflammation in joints, ligaments, and tendons
- Helping prevent systemic health problems like diabetes and heart disease, which can have harmful effects on your feet
Healthy Changes
Unfortunately, for many Douglas Park/Los Angeles County area patients, eating healthy seems like deprivation. However, many changes can be painless and even enjoyable. Try some of the tips below and aim to incorporate more nutritious choices into your menus slowly. Create more colorful plates. Eating a rainbow of different kinds of produce will help ensure that you are getting a well-rounded variety of vitamins, minerals, and antioxidants into your diet.
- Cook more meals at home. Make it a family affair and involve your children in meal planning, shopping, and preparation.
- Travel the world through your menus, at home and in restaurants, sample the wide variety of healthful cuisines available from other countries. Don’t be afraid to experiment with new spices and cooking methods like roasting and steaming the preserve nutrients without adding fat or high-calorie ingredients.
- Eat seasonally. Fruits and vegetables that are in season or, better yet, locally grown are going to be fresher, more nutritious, and delicious. Consider joining a CSA (Community Supported Agriculture) and learn about the growing season in your part of the country.
Eating a nutritious diet is just one way to be proactive in the health of your feet. If you want to learn more or you are currently experiencing any lower extremity discomfort, make an appointment to see our podiatrists, Dr. Victoria M. Foley and Dr. Constance Ornelas, by calling our Long Beach office for an at (562) 420-9800.
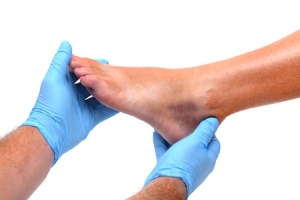
6 Signs You Need to Call the Foot Doctor
At Superior Foot & Ankle Center we find that many patients do not fully realize the role the podiatrist can play in your foot and overall health. Our purpose is to provide acute and preventive care to your entire lower extremity (from the tips of your toes up to your knees). We have a wealth of treatment options available including pain relief, multiple therapies, custom orthotics, exercise and surgery to correct and improve foot discomfort associated with both age and activities, including sports injuries. In addition, in many cases the foot doctor is able to diagnose a larger, systemic issue from symptoms in your feet and can then collaborate with other health care professionals to care for the disorder.
Use the following as a guideline if you’re trying to decide if you should call the podiatrist:
- You experience sudden or increasing pain; chronic pain seems to be getting more severe or more frequent
- You notice abnormalities in your feet: swelling, changes in shape or size, bruising, lumps,
- Other non-painful symptoms: tingling, burning, itching, pins and needles, numbness
- Changes in skin (color, redness, scaling, flaking, sores, blisters, cracking) or toenails (discoloration, thickening, crumbling, peeling)
- Possible signs of infection: pus or discharge, redness or red streaks, tenderness, heat, fever
- You have any symptoms and have diabetes or other conditions that suppress the immune or circulatory systems—even the most minor symptoms can become major medical threats to these patients
If you said yes to any of the above symptoms or signs, contact our Long Beach office for an appointment by calling: 562-420-9800. Our foot and ankle surgeons, Dr. Victoria Foley and Dr. Constance Omelas will do a complete examination and help get to the bottom of your foot pain so that you can get back to the active lifestyle you love. Regardless of whether your foot disorder is common, such as athlete’s foot or an ingrown toenail or a more complex condition, starting treatment sooner rather than later will enable the foot doctor to use the least invasive methods and ensure the quickest cure.
Protect Your Feet While Playing Sports
How To Protect Your Feet While Playing Sports
Anyone who has played sports knows just how strenuous it can be on your feet. Think of all the skilled movements you make as an athlete: the swift twists and turns in basketball, the rigorous sprints taken in a football or baseball game, and the hard landings made after a volleyball spike. Regardless of how fit you are, the physical demands of your sport will still leave you stepping off the court or field with sore, tired feet.
Considering the wear and impact a sport can take on your feet, there is always the likelihood of damage or injury. In order to keep yourself in top condition to compete, proper foot care is essential.
Proper Footwear
Footwear appropriately designed for the sport is essential to prevent injury. A common bad habit among pickup players is wearing running shoes or skate shoes, even in a high-impact sport like basketball or volleyball.
Skate shoes are a horrible choice for any non-skating sport: they have extremely flat soles, designed to grip a board as tightly as possible. But for any other sport, you will not have the proper arch support or cushioning required for your movements.
While running shoes are perfectly appropriate for a casual game of football or soccer at the park, they are a poor choice for a sport like basketball. They may have the proper cushioning needed for running down the court, but they do not have a sole designed to grip the court surface when playing defense, increasing the likelihood of slipping. Moreover, they have neither the cushioning nor the ankle support to allow for a safe landing in basketball or indoor volleyball. Even popular low-top basketball shoes like the Kobe series will support your ankles better than a pair of running shoes.
Using either of these shoes improperly will put you at risk for conditions like plantar fasciitis or a serious ankle injury. It may not be possible or practical to have the perfect shoe for every activity, but make sure to choose the safest option available. For example, a basketball shoe would also be appropriate for court or concrete volleyball, since both sports involve quick movements, jumping, and hard landings.
Protecting Against Specific Injuries
If you have had an injury before, you know exactly which parts of your body are weaker and more prone to injury. Consider purchasing a brace or other type of support to protect your vulnerabilities.
General Precautions
- Take time off from your sport to recover, at least one day a week.
- Wear the proper equipment, such as pads (neck, shoulder, elbow, chest, knee, and shin), helmets, mouthpieces, face guards, protective cups, shoes, and/or eyewear. It’s worth mentioning that these will not guarantee safety, but they help immensely.
- Do strength and conditioning before playing. Fatigue is one of the top ten causes of injury.
- Increase your flexibility by stretching daily, and before and after games as well.
- Utilize the proper form and technique, for everything from throwing, shooting, kicking, blocking, and footwork.
- Take breaks in the middle of your game or practice session. This will reduce the chance of injury due to fatigue, as well as heat-induced illness.
- Play safe. Penalties and regulations in sports exist for a good reason.
- Do not try to be tough: stop playing if you notice pain.
- Drink plenty of fluids before, during, and after physical activity. Dehydration can lead to cramping (especially in the legs and feet), severe headaches, and heat injury.
- Wear light clothing.
- Wear breathable shoes to prevent foot conditions like toenail fungus.
The Trusted Podiatrist of Athletes
Whether you are a serious competitor on a sports team, or a casual player who loves to play pickup games on the weekend, a dedicated podiatrist who prioritizes your foot health is essential.
If your hobbies have been hard on your feet, schedule a consultation today with esteemed podiatrist Dr. Vikki. Dr. Vikki has a reputation as the trusted choice of Special Olympic athletes, and an outstanding record of patient satisfaction.
For this and all your related foot care concerns, contact the specialists at Superior Foot & Ankle Care Center today.
Treating Bone Spurs
How to Treat Bone Spurs
Have you been experiencing a sharp pain in your foot, but you can’t figure out why? Chances are that you have developed a condition called bone spurs.
A bone spur is a small bony growth or a collection of growths which form on joints like the spine, shoulders, hands, hips, knees, and the feet. While we will be focusing on the feet, much of the information below will apply to bone spur treatment in general:
Bone Spurs: Causes
A bone spur occurs when the body attempts to repair itself by building extra bone on areas affected by long periods of pressure, rubbing, or stress.
Bone spurs rarely cause pain on their own. If they grow on the feet, however, calluses may form to cushion the affected area. As the wear and tear on the joints continue, the spurs may compress the surrounding ligaments, tendons, or nerves. This results in injury to the surrounding tissue, in addition to swelling, pain, and tearing.
There are several factors which may contribute to a bone spur. The aging process is partly to blame: cartilage, which covers the ends of bones in a joint, slowly wears away due to a process called osteoarthritis. The damage to the joints will lead to pain and swelling, and will often result in a bone spur. Osteoarthritis is a common cause of bone spurs in joints of the feet and spine.
Tight ligaments will also make you more vulnerable to bone spurs. Many factors can cause this tightness, including strenuous activities which affect the feet like dancing, running, long periods of walking, basketball, and tennis. Other factors include:
- Obesity: excess weight will result in excess pressure on the feet.
- Tight-fitting shoes (like high-heels) can put undue pressure on the feet, causing stress and tightness in the foot, particularly in the heel. Shoes which lack proper arch support, like worn-out shoes, can worsen this problem as well.
- Plantar fasciitis, an inflammation of the plantar fascia ligament. Repeated stretching and tearing of the plantar fascia and other muscles in the feet can lead to increased wear and tear on the heel.
- Abnormalities in walking.
- Diabetes.
- Occupations which require long periods of standing.
- Flat feet or high arches.
Bone Spurs: Treatment
Bone spurs rarely require treatment, unless they cause frequent pain or damage to surrounding tissues. Unless these symptoms are present, it is difficult to detect a bone spur without an X-ray (though it is rare to use an X-ray for this condition, since it rarely causes symptoms). Since heel spurs and plantar fasciitis are closely related, many of the same treatment methods for plantar fasciitis will be used for bone spurs as well. Consider these tips to find relief:
- Resting from the activity causing the bone spur will be recommended. If it cannot be avoided (due to an occupation, for example), ice the affected area immediately after the activity is finished.
- If you have a heel spur, warming up before a strenuous activity and stretching the calf muscles may also be helpful. These stretches will gently lengthen the calf muscle, relaxing the tissue surrounding the heel. Commit to stretching several times throughout the day, particularly in the morning and after a prolonged period of sitting or standing, when the muscles in the feet are stiffest.
- If osteoarthritis or plantar fasciitis are causing pain or damage, weight loss will reduce pressure on the joints and mitigate symptoms.
- Learn how to take proper care of your joints.
- Visit a physical therapist to have an ultrasound or deep tissue massage, especially if your pain is related to plantar fasciitis.
- Wear shoes with good arch and heel support. Try using an orthotic insert in your shoe, to add more support or padding for a corn or callus.
- A doctor may prescribe a corticosteroid injection to reduce pain and inflammation. This will be more of a last resort, since side effects may exacerbate symptoms, especially with heel spurs.
- Discuss surgical removal of the bone spur, which will loosen the plantar fascia.
Consult the Experts
Bone spurs are difficult to detect, and the volume of potential variables related to foot pain can make it difficult to determine the cause. If you’re suffering from foot pain, schedule your consultation with expert podiatrist Dr. Vikki today. Dr. Vikki has a reputed record of patient satisfaction, and is the trusted podiatrist of Special Olympic athletes.
For this and all related foot care concerns, the caring professionals at Superior Foot & Ankle Care Center are happy to help with your podiatric needs.
Home Plantar Wart Treatment
How To Treat Plantar Warts At Home
A plantar wart is one of just a few soft tissue conditions, which can be very painful. It is also very common, and can be treated at home with common household items or over-the-counter products.
Treating Plantar Warts: Causes and Symptoms
Plantar warts are caused by a virus which invades the skin through small or even invisible cuts and abrasions. It is most often contracted while walking barefoot on dirty surfaces or littered areas.
Communal bathing facilities and other warm, moist environments are also breeding grounds for the virus.
Plantar warts are found on the bottom of the feet. They tend to be hard and flat, with a rough surface and defined boundaries. They are often gray or brown (colors may vary) with one or more pinpoints of black. Left untreated, the warts may grow to an inch or more and may even spread into clusters (often called mosaic warts).
These warts are very resistant to treatment, and may even return after healing; but some have been known to disappear on their own. Though warts may be painful on weight-bearing areas of the feet (e.g. the ball of the foot or the heel), most warts are harmless.
Read more about warts and how to identify them here.
Plantar Wart Treatments: Home remedies
Peeling Medicine
Nonprescription wart removal methods typically come as a patch or liquid. The directions usually tell patients to wash the affected area and soak it for 20 minutes. Gently remove the dead tissue with a pumice stone or emery board, then apply the solution or patch. Patches are typically changed every 48 hours, while liquid applications are applied twice a day. Results may not appear for several weeks.
Cryotherapy
You may be able to get this kind of treatment from the doctor . The doctor will trim the wart with a small knife. In rare cases, local anesthetic may be administered. Then, the doctor applies liquid nitrogen with a probe or cotton swab.
Duct Tape
For this method, cover the wart with silver duct tape for six days, then soak the wart in water. Remove the dead tissue with a pumice stone or emery board, and leave the wart exposed for 12 hours. Repeat this process until the wart is gone. Keep in mind that this method has seen mixed results at best.
You may want to discuss these methods with your doctor first. Most over-the-counter wart treatments will contain acids or chemicals which destroy skin cells. An expert hand will be able to destroy the abnormal skin cells without harming the surrounding healthy tissues. Patients with diabetes, cardiovascular diseases, or circulatory disorders should avoid self-treatment entirely.
Prevention
There are a few steps to take in order to prevent plantar warts from forming:
- Avoid direct contact with warts, including your own.
- Keep feet clean and dry, and change shoes and socks daily. This basic step is essential for preventing blisters and fungal infection as well.
- Wear shoes or sandals in areas where the wart virus thrives, such as communal showers, dirty areas, and swimming and pools.
- Don’t pick at the warts, as this may cause the virus to spread.
Reserve a different pumice stone or emery board for the warts, and another for healthy skin and nails. - Use a disposable emery board to avoid spreading the virus
Wash hands thoroughly after touching a wart. - Check children’s feet regularly.
When To See a Doctor
If you have a plantar wart and the treatments listed above haven’t been effective, you should see a doctor about other treatment options. Generally, it is always a good idea to see a doctor whenever there is a growth or eruption on the feet to ensure the correct diagnosis. Sometimes, what appears to be a wart may actually be a sign of cancer – for example, carcinoma or melanoma.
Ask the Experts
If you are concerned about a wart that won’t go away, schedule an appointment with Dr. Vikki or Dr. Connie today. For more foot care advice, contact the specialists at Superior Foot & Ankle Care Center.
Preventing Ingrown Toenails | Superior Foot & Ankle Care Center
How to Prevent Ingrown Toenails
While an ingrown toenail might happen to some people more than others due to hereditary factors, the fact is that an ingrown toenail can happen to anyone. Simply put, an ingrown toenail occurs when a nail grows into the flesh rather than over it, occurring most often in the big toe. The nail will irritate the skin, causing pain and even infection should it break into the skin. (An infected ingrown toenail will be red, swollen, hot, and painful). Ingrown toenails can become very painful conditions, but only because patients are often unaware of what the condition is and how it occurs.
Causes of Ingrown Toenails
A number of factors might cause an ingrown toenail:
- Wearing shoes that are too small. This is most common among teenagers.
- Hereditary traits like thick or curved nails will make a person more prone to ingrown toenails.
- Socks that are too short or tight will force the toes toward each other and encourage the nails to grow into the skin.
- Athletic people are also more prone to ingrown toenails. Excessive sweating makes the skin and nails softer and easier to split. Those split nails can easily puncture the skin.
- Trauma – such as stubbing, jamming, or dropping something on a toe – can contribute to the development of ingrown toenails.
- Active people who participate in activities like running, soccer, or ballet will need to be pay special attention to the signs of an ingrown nail.
- A common cause of ingrown toenails, improper nail trimming will encourage the skin to fold over the nail.
How to Treat an Ingrown Toenail
If caught in its early stages, an ingrown toenail may be prevented or even cured by taking the following steps:
- Soak the affected toe in water for 10 minutes. This will soften the folds of skin around the nail.
- Using a Q-tip, push the skin fold over the ingrown nail down and away from the nail. Start at the root of the nail, then move toward the end of the nail.
- Repeat every day for a few weeks and allow the nail to grow.
- Once the nail has grown forward far enough, place a tiny piece of cotton wool or dental floss under it. This will prevent the nail from growing into the skin. Change the wool or floss every day after soaking the foot.
- Continue to let the nail grow forward until it is over the end of the toe. Cut the nail straight across – not rounded off at the ends.
Generally, persistent and troublesome symptoms should be brought to a doctor’s attention. The situation becomes urgent if the patient has diabetes or a poor immune system, since the infections must be treated immediately.
Patients with diabetic neuropathy, peripheral arterial disease, or those who have otherwise lost the nerves or feeling in their feet should see a doctor ASAP.
Additionally, patients that take are on chemotherapy or any immunosuppressant medications must see a doctor immediately.
These conditions make it difficult to sense problems like deep infections, requiring monitoring and assessment from a podiatrist.
Preventing Ingrown Toenails
- Cut nails straight across, being especially careful not to cut too short or low at the sides. The corners of the nails should be visible above the skin. Cutting nails after a shower is easiest, since the nails are softer.
- People who see a pedicurist should ensure that they are trimming straight across.
- Patients with poor blood flow may not be able to trim their nails on their own, and should therefore see a podiatrist regularly for trimming.
- Toenails should be kept even with the tips of the toes. Trim too short, and pressure from shoes might lead the nail into the tissue.
- Wear shoes that fit properly. People with nerve problems or chronic ingrown toenails may need to visit a shoe store that specializes in people with foot problems.
- Wear protective footwear, especially in a warehouse or other environment where foot injuries are common.
Keep feet clean and dry, and air them out as much as possible. - Avoid tight shoes. Use cotton socks and not synthetic.
- Diabetics must take extra care when cutting nails, and pay special attention for the symptoms of ingrown toenails.
- Cut the nails straight across, following the shape of the toe. Do not cut too low at the sides.
- Gently file away sharp edges.
- See a podiatrist for nail trimming if loss of feeling in the feet occurs.
- Patients with poor vision should see a chiropodist to trim their nails.
For more information about feet and nails, or to schedule an appointment, please visit Dr. Vikki.
Changing Your Shoes for the New Season
It is very important to have shoes that have just the right amount of arch support, particularly for those who transition into boots during the winter time. Seasonal Footwear all have their own unique support issues. Most boots lack the cushion and support that sneakers have while summer sandals do not provide proper ankle support.
Wearing appropriately-fitted shoes is a key part of keeping your feet healthy and in working order. You need shoes with good arch support and stable shoes, but it can be difficult to find the footwear that provides the best orthopedic fit for your feet. Without proper arch supports you leave yourself open to developing pain in your heels, ankles, knees and even lower back.
Dr. Foley and Dr. Ornelas of Superior Foot & Ankle Center have compiled a list of shoes and shoe retailers that are best suited to prevent a variety of foot-related injuries and issues. This list separates shoes by athletic categories, such as running, cross-training, basketball, hiking and golf. To avoid these problems you should always find shoes that have just the right amount of arch support or else wear orthotic insoles.
Here’s some information about what orthotics are and what different kinds are available.
What are Orthotics?
Orthotics are inserts that correct a number of foot-related problems from flat feet to heal pain. While they do not fix any major biomechanical problems with your feet, they do provide relief for minor aches and pains.
Over the Counter Orthotics
There are a number of different kinds of over-the-counter orthotics that treat minor foot problems and alleviate pain. For example, arch supports can help correct fallen arches or flat feet while gel inserts help relieve foot and heel pain.
Prescription Orthotics
If you find that over-the-counter orthotics are not alleviating your pain, and it is best to consult a foot care professional about getting prescription orthotics. Prescription orthotics are high-quality inserts that address your specific foot care needs. These custom orthotics correct any number of serious foot problems from plantar fasciitis to abnormal motion. In addition, custom orthotics can relieve severe pain in your feet, knees, shins and back. They can even be used to help diabetic treat their painful foot ulcers and calluses. Prescription Orthotics are created by taking a mold or scan of your feet, so you know that your individual foot issues are being addressed.
Other Things You Should Know
You can find orthotics that are designed to fit and work inside high heel shoes.
Because over the counter orthotics can take a while to break in it is best to wear them around the house for a few days before wearing them to work. Many shoe brands come with extra padding and support. For example Cole Haan dress shoes and boots all come with Nike Air inserts.
Over the counter inserts can last anywhere from 3 months to a year, depending upon how much standing and walking you do at your job. For this reason, people with jobs that require a lot of standing and walking such as nurses and waitresses should have a spare pair of inserts just in case.
Now that you know the importance of having proper foot support in all of your shoes no matter what season it is, be sure to use orthotics to correct and prevent pain. If you are experiencing foot pain, no matter how minor, it is important to speak to a foot care professional as soon as possible to discuss ways to correct this issue. If you have any questions about orthotics; please feel free to contact us today to schedule a consultation.
Treating Blisters Without Your Doctor’s Help
Treating Your Blister
Although most blisters eventually heal on their own, the recovery time required isn’t a feasible option for those who are active or experiencing pronounced pain. It is important to know the right methods of treatment to remain healthy and to prevent your blister from getting worse.
What Causes a Blister?
Blisters occur when temperatures rise, causing the feet to swell and sweat. This results in additional friction formed between the feet and shoes, creating a fluid-filled sac around the affected area.
Treating An Unbroken Blister
The treatment method depends on where the blister is located and its level of severity. An unbroken blister or a blood blister will heal on its own. All that is required is a bandage to protect it, and avoidance of the activities which caused or may aggravate it.
For a small blister on a weight-bearing area (such as the heel, or the ball of the foot a doughnut-shaped felt pad should be applied. Leave the area above the blister open as much as possible.
In most cases, popping a blister at home is not advised. If it is too painful, however, follow these steps to drain it safely:
- Wash both your hands and the blister with soap and warm water.
- Swab the blister with iodine.
- Take a needle or a straight pin and wipe it with rubbing alcohol.
- Gently puncture the edge of the blister.
- Press the fluid toward the hole to drain it out.
Never drain a blister, no matter how small it may be, if the following is true:
- You have diabetes, cancer, HIV, heart disease, or another condition which increases the risk of infection.
- You have reason to believe that the blister was caused by a contagious disease, such as chickenpox. If you drain this type of blister, the virus may spread to other people.
Treating a Torn (Or Drained) Blister
Once the blister has torn or drained, follow these steps:
- Wash the area with soap and water – not alcohol, iodine, or any other cleanser.
- Leave the flap of skin over the blister, unless there is dirt or pus under it. Smooth the flap over the exposed layer of skin.
- Apply antibiotic ointment such as Bacitracin or Triple antibiotic ointment and then a clean bandage. If an itch or rash develops, discontinue the ointment, since there may be a skin reaction.
- Change the bandage whenever it becomes wet or dirty, and remove it every night so the affected area can dry. If you are going to remain active as the blister heals, you may find Band Aid blister cushions or 2nd Skin blister pads particularly helpful.
When To Call a Doctor
Call your doctor if the following occur:
Monitor the area closely for signs of an infection. These may include: increased pain, swelling, redness, or warmth surrounding the blister; red streaks extending from the blister; drainage of pus; or fever.
Call your doctor if you notice these symptoms:
- A crusty blister which drains honey-colored fluid.
- Signs of illness, such as shaking chills, fever, belly pain, vomiting, diarrhea, muscle or joint aches, headaches, or a vague sense of illness.
- Symptoms do not improve, or increase in severity and/or frequency.
Preventing Blisters
Since blisters are caused by the friction between your feet and your shoes, wear shoes that fit well. This means that you should be able to wiggle your toes inside the shoe. Your feet swell later in the day, so try on shoes in the afternoon or the evening.
Moisture-wicking socks help reduce the swelling of the feet and friction associated with blisters. There are other socks and insoles designed to prevent blistering as well.
Applying moleskin to an area of the shoe where your feet rub may also help. Dust the inside of your shoe with talcum powder.
Avoid contact with plants like poison ivy, oak, or sumac.
Avoid contact with people who have infections that can cause blisters, such as:
- Viral illness like chickenpox, shingles, genital herpes infection, and cold sores
- Bacterial skin infection
- Scabies mite infection
Ask the Expert
To learn more about keeping your feet healthy, read the 15 Steps to Fabulous Summer Feet.
For the best in foot care, schedule an appointment with specialist Dr. Vikki or Dr. Connie at the Superior Foot & Ankle Care Center today.
Does Your Foot Pain Signal a Serious Condition?
You might be surprised to learn that many diseases have foot pain as one of their symptoms. Problems with the thyroid can cause nerve sensations in the feet; or degeneration in the lower back might irritate the nerves of the spine, impeding sensation in the feet. Learning what signs to look for could improve your life or even save it.
Peripheral Arterial Disease (PAD)
PAD occurs when plaque – a fatty substance which builds up in the arteries in the legs – reduces blood flow to the lower legs and feet. Symptoms include cramping in the calves, or other parts of the leg while it is in motion. It may even cause foot pain, or prevent wounds in the foot from healing properly.
While the most obvious symptoms of PAD involve the legs, it is associated with hidden damage to the heart and brain. This means that PAD sufferers are at a higher risk of heart attack and stroke. Smoking, diabetes, high cholesterol, and high blood pressure will also increase the risk of PAD. Medications may be prescribed, but diet and lifestyle changes are also necessary.
Rheumatoid Arthritis (RA) and Gout
The Arthritis Foundation revealed that 46 million Americans have arthritis or other chronic joint problems. Of the 1.3 million Americans who suffer from rheumatoid arthritis, 90 percent of them will experience symptoms in their foot and ankle.
RA develops when the body’s immune system mistakenly attacks the joints, causing pain and swelling. If RA reaches the feet, pain will begin in the toes, and then spread to the feet and ankles later on. The joint damage caused by RA can even change the shape of the toes and feet, given enough time. RA treatment involves medication, exercise, and sometimes surgery.
Gout is another type of arthritis caused by the accumulation of uric acid in the body. The acid collects in the joints, especially the big toes, and will cause intense, episodic pain. The acid may even cause kidney stones if it builds up there.
Gout treatment involves exercise, lots of water, avoidance of certain medications, and staying at a healthy weight. Doctors may prescribe gout patients with nonsteroidal anti-inflammatory drugs (NSAIDs), steroids, or other medications.
Diabetes
Approximately 24 million Americans have diabetes, but 6 million don’t even know it. Diabetes is a condition in which glucose, or blood sugar, builds up in the blood. While glucose is necessary to fuel the body, an excess amount will damage nerves and blood vessels in the feet, causing decreased sensation and reduced blood flow.
Other symptoms of diabetes include numbness and tingling in the feet, and severe foot infections. While many people experience foot discomfort after a long day of standing, severe foot pain out of proportion with your activity level is a problem that should be reported to your doctor. Diabetes can lead to other major foot problems as well, and possibly surgical removal of the toe, foot, or lower leg.
Diabetes can be treated with medication and regular foot exams. It also requires lifestyle changes like quitting smoking, and wearing supportive shoes to mitigate foot trauma.
For more information on foot pain or to schedule an appointment, contact Superior Foot & Ankle Care Center.
How Treat and Prevent Foot Blisters
Blisters are common, especially for those who do a lot of walking or running. However, many people don’t know how to care for their blisters properly. Here are some tips for healing any blisters you may already have, and how to avoid new ones from forming:
When You Can Remove a Blister
When blisters are small and do not show any signs of infection, it is perfectly okay to pop them. Simply disinfect the area and drain before the blister can become infected. Afterward, treat the wound with antibiotic ointment.
To safely pop your blister, you should:
- Thoroughly wash your hands and the blister with water and antibacterial soap. Then cleanse the blister with rubbing alcohol or iodine.
- Gently rub your blister to see if it will pop on its own. If it doesn’t, soak your feet in warm water for 30 minutes. Then try popping it again.
- Cover the wound with antibiotic ointment and a bandage.
When You it Shouldn’t Be Remove
If your blister shows signs of redness, swelling, soreness, pus, or even pain, do not pop it. All of these symptoms may indicate that you have a serious infection, or that your blister is actually a foot ulcer. Both of these conditions require the attention of a podiatrist to be treated properly. Foot ulcers, particularly for diabetics, can become gangrenous and result in the need for amputation. If you are experiencing any of these symptoms, or if you suspect that you have a foot ulcer, seek medical attention immediately.
Blister Treatment
Blisters are often sore while they are healing, so be sure to keep your feet comfortable. For example, put extra padding on the affected area, or use a healing ointment that also provides pain relief.
Blister Prevention
In order to prevent future blisters, make sure that you always wear shoes that fit properly. In addition, avoid going sock-less while wearing shoes like sneakers or boots, particularly if you’re going to be walking for a while. When you do wear socks, be sure that they are thick and provide extra padding in sensitive area like the back of the heel. Cotton socks absorb moisture, causing blisters when the wet socks rub against your feet.
People with foot abnormalities, such as bunions, often develop blisters. If you are constantly suffering from blistering feet, consult your foot care professional.
For more foot care tips and tricks, consult the experts at Superior Foot & Ankle Care Center with all of your podiatric questions and concerns.